What is PMH (Past Medical History) in Healthcare?
PMH (Past Medical History) refers to the documented record of a patient’s prior medical conditions, diagnoses, hospitalizations, surgeries, and significant health events that occurred before the current episode of care. PMH provides essential historical context that informs clinical decision-making and risk assessment.
In healthcare workflows, PMH is a core component of Hx (History) and plays a critical role in shaping Dx (Diagnosis), guiding Tx (Treatment), and informing care planning from SOC (Start of Care) through DC (Discharge). PMH helps clinicians understand baseline health status, anticipate complications, and avoid redundant or inappropriate interventions.
PMH is typically collected during intake, initial assessment, or as part of the H&P (History and Physical) and is referenced throughout the episode of care. In Medicare-regulated and post-acute settings, PMH documentation supports medical necessity by explaining why a patient may require a certain level of care, longer LOS (Length of Stay), or interdisciplinary involvement.
Because PMH influences so many downstream decisions, accuracy and completeness are critical. Missing or outdated PMH can lead to misaligned care plans, documentation gaps, and increased compliance risk.
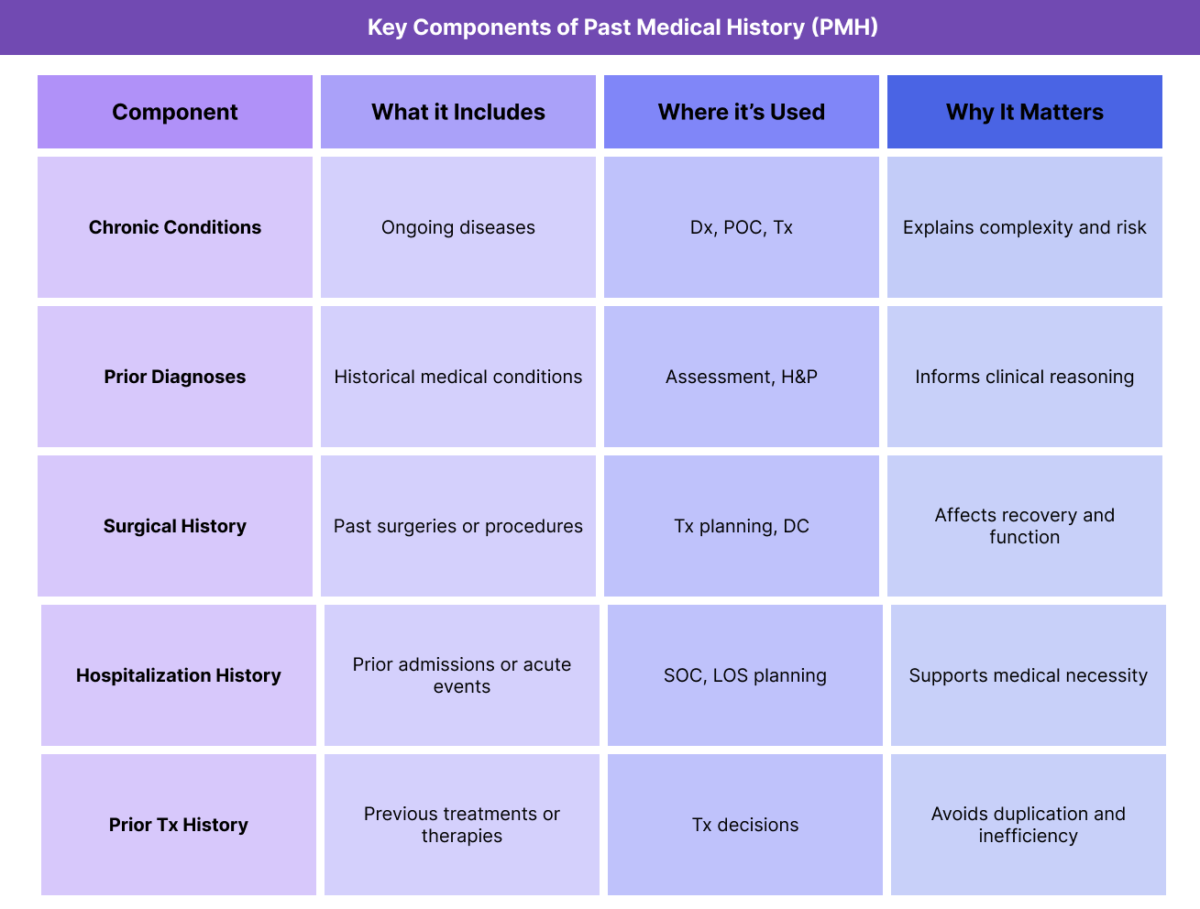
Key Components of Past Medical History (PMH)
PMH is composed of several distinct but interrelated elements that together describe a patient’s prior health experience.
Chronic Medical Conditions
Chronic conditions such as diabetes, heart failure, COPD, or hypertension are central components of PMH. These conditions often influence current symptoms, treatment options, and risk during care delivery.
Documented chronic PMH frequently explains care complexity and ongoing need for services.
Prior Diagnoses and Significant Illnesses
PMH includes resolved or historical diagnoses that may no longer be active but still affect clinical reasoning. Prior cancers, strokes, or major infections often remain relevant even after resolution.
Surgical and Procedural History
Past surgeries and procedures provide insight into anatomical changes, recovery limitations, and potential complications. Surgical PMH often influences mobility, ADL performance, and discharge planning.
Prior Hospitalizations and Acute Events
Recent or recurrent hospitalizations, emergency visits, or acute exacerbations are key PMH elements, particularly in post-acute and transitional care settings.
These events often explain why care was initiated at SOC.
Long-Term Treatments and Therapies
PMH may include prior Tx (Treatment) such as long-term medication use, therapy programs, or disease management interventions. Understanding prior treatment response helps tailor current care.
How Past Medical History (PMH) Works in Practice
PMH is actively used throughout the care episode to support safe, effective, and compliant care.
Collecting PMH During Intake and Start of Care (SOC)
PMH is commonly collected during intake or at SOC (Start of Care) through patient interviews, referral documentation, prior records, and caregiver input. Early PMH accuracy is critical because it shapes initial Dx and the POC (Plan of Care).
Incomplete PMH at SOC can result in misaligned care planning.
Using PMH to Support Diagnosis (Dx)
PMH provides context that helps clinicians interpret current symptoms and assessment findings. Prior conditions often clarify whether symptoms represent new issues, exacerbations, or expected progression.
Accurate PMH strengthens Dx justification.
Leveraging PMH for Treatment (Tx) Planning
PMH informs Tx (Treatment) selection by highlighting contraindications, prior response to therapy, and long-term management needs. Clinicians use PMH to avoid repeating ineffective interventions.
Sharing PMH Across the IDT
PMH must be accessible to the IDT (Interdisciplinary Team) to ensure coordinated decision-making. Fragmented PMH documentation can lead to inconsistent or duplicative care.
Referencing PMH Throughout LOS and at Discharge (DC)
During LOS (Length of Stay), PMH helps contextualize progress and setbacks. At DC (Discharge), PMH informs follow-up planning, referrals, and patient education.
PMH in Billing, Medical Necessity, and Documentation Oversight
While PMH (Past Medical History) is not billed directly, it is a critical supporting element in how payers evaluate medical necessity, episode complexity, and appropriateness of care—particularly in Medicare-regulated and post-acute settings.
How PMH Supports Medical Necessity
Medical necessity is evaluated in context, not in isolation. PMH provides that context by documenting a patient’s baseline health status, chronic conditions, and prior acute events. This background helps explain why certain services, visit frequencies, or interdisciplinary involvement are required.
For example, a patient with extensive PMH may reasonably require a longer LOS (Length of Stay) or more intensive Tx (Treatment) than a patient with fewer comorbidities. Without documented PMH, that care may appear excessive during review.
PMH and Reimbursement Integrity
Accurate PMH documentation helps ensure reimbursement reflects patient complexity. Chronic conditions, prior hospitalizations, and surgical history often explain why care is more resource-intensive.
Incomplete PMH can lead to:
- Understated patient risk
- Misaligned care planning
- Reimbursement that does not reflect true care needs
Conversely, unsupported PMH entries increase audit risk.
PMH in Episode-Based and Transitional Care Models
In episode-based and transitional care models, PMH informs expected utilization and outcomes. Payers may evaluate whether services delivered from SOC (Start of Care) through DC (Discharge) align with what would reasonably be expected given the patient’s documented history.
Common PMH-Related Documentation and Compliance Risks
PMH-related issues typically arise from documentation quality rather than clinical intent.
Common risks include:
- PMH not fully collected at SOC
- Outdated PMH not revised during care
- PMH inconsistencies across H&P, SOAP, and progress notes
- PMH not clearly connected to Dx or Tx
- Copy-forward PMH without verification
Auditors often question care decisions when PMH does not support documented services.
System and Workflow Challenges Affecting PMH
PMH quality is heavily influenced by system design and workflow execution.
Fragmented PMH Across Records
When PMH is split across multiple systems or buried in narrative notes, clinicians may lack full visibility into patient history. Fragmentation increases the risk of errors and misaligned care.
Limited Time for PMH Collection
Time constraints during intake or SOC can result in partial PMH capture. Without structured follow-up workflows, gaps may persist throughout LOS.
Poor Accessibility for the IDT
If PMH is not easily accessible to the IDT (Interdisciplinary Team), care decisions may be made without full historical context, reducing coordination and effectiveness.
How PMH Influences Quality, Access, and Equity
PMH plays a direct role in patient outcomes and fairness in care delivery.
PMH and Quality of Care Outcomes
Accurate PMH supports safer, more targeted care. Understanding prior conditions and treatments helps clinicians anticipate complications, tailor Tx, and set realistic goals.
Poor PMH documentation can lead to inappropriate interventions or missed risks.
PMH and Access to Healthcare Services
PMH often influences eligibility and authorization decisions. Missing or unclear history can delay enrollment, services, or transitions—especially at SOC or following discharge from another setting.
Equity Considerations in PMH Documentation
Social factors, access to prior care, and health literacy can affect how completely PMH is reported. Patients from underserved populations may have fragmented records or limited ability to recall history.
Equity-aware PMH practices involve verification, clarification, and culturally sensitive communication to ensure history is accurately captured.
Frequently Asked Questions about PMH in Healthcare
1. What does PMH mean in healthcare?
PMH stands for Past Medical History and refers to a patient’s documented history of prior medical conditions, diagnoses, hospitalizations, surgeries, and significant health events. PMH provides essential context for clinical decision-making and care planning.
2. How is PMH different from Hx (History)?
Hx (History) is a broad category that includes multiple elements such as PMH, medication history, social history, and family history. PMH is a specific subset of Hx focused solely on prior medical conditions and events.
3. Where is PMH documented in the medical record?
PMH is typically documented during intake, at SOC, or as part of the H&P (History and Physical). It may also be referenced throughout progress notes, SOAP documentation, and discharge summaries.
4. Why is PMH important for Medicare compliance?
In Medicare-regulated programs, PMH helps establish medical necessity by explaining patient complexity and risk. Reviewers often evaluate PMH when determining whether the level and duration of care were appropriate.
5. Does PMH need to be updated during an episode of care?
Yes. PMH should be reviewed and updated as new diagnoses, hospitalizations, or significant events occur. Keeping PMH current ensures care decisions remain aligned with the patient’s true health status.
6. Can incomplete PMH affect audits or payment?
Yes. Incomplete or inconsistent PMH can weaken documentation and raise questions about necessity, potentially leading to audits, denials, or delayed payment.
7. How does PMH relate to CC, ROS, Dx, and Tx?
PMH provides background context that supports interpretation of the CC (Chief Complaint) and ROS (Review of Systems), informs Dx (Diagnosis), and guides Tx (Treatment) decisions. Consistency across these elements strengthens the clinical narrative.
