What is the National Correct Coding Initiative (NCCI)?
The National Correct Coding Initiative (NCCI) is a set of coding policies and automated claim edits developed by the Centers for Medicare & Medicaid Services (CMS) to prevent improper billing of services that should not be reported together. NCCI is primarily used in Medicare fee-for-service but also influences Medicare Advantage and other payer coding rules.
In practice, NCCI edits are applied during claims processing to identify code combinations that represent duplicate, mutually exclusive, or overlapping services. When an invalid combination is detected, the claim may be denied or require a modifier to indicate that services were distinct and separately reportable.
From an operational standpoint, NCCI is a core driver of coding accuracy, denial prevention, and compliance risk. Many denials attributed to “coding errors” are actually NCCI edit failures, making NCCI understanding essential for billing teams, compliance leaders, and healthcare technology vendors.
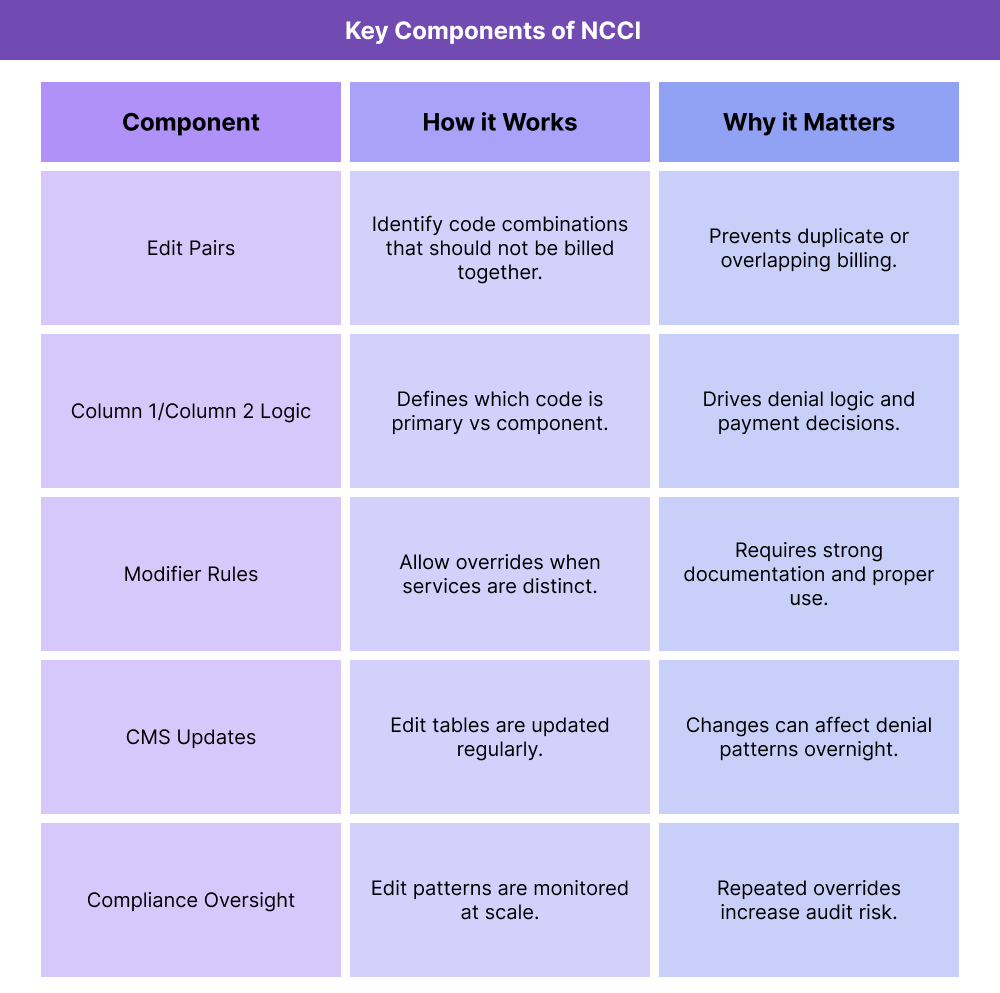
Key Components of the National Correct Coding Initiative (NCCI)
NCCI is built around structured edit logic that determines whether CPT and HCPCS codes can be billed together. These components explain how NCCI works and why it matters operationally.
NCCI Edit Pairs and Code Combinations
At the heart of NCCI are procedure-to-procedure (PTP) edit pairs. These edits identify code combinations where one service is considered a component of another or where two services are mutually exclusive.
When both codes in an edit pair are billed together, Medicare will generally deny payment for the secondary code unless an appropriate modifier is used and supported by documentation.
Column 1 / Column 2 Code Logic
NCCI edit pairs designate a Column 1 code (the more comprehensive service) and a Column 2 code (the component or lesser service). By default, only the Column 1 code is payable.
Understanding which code is Column 1 versus Column 2 helps billing teams anticipate denials and apply modifiers correctly when appropriate.
NCCI Modifiers and Override Rules
Certain NCCI edits allow the use of modifiers—most commonly modifier -59 or related modifiers—to indicate that services were distinct and separately reportable.
Operationally, this requires:
- Clinical documentation that clearly supports distinct services
- Appropriate modifier selection
- Avoidance of routine or blanket modifier use
- Improper modifier use is a common audit and compliance risk tied to NCCI enforcement.
NCCI Edit Tables and CMS Updates
CMS updates NCCI edit tables on a regular schedule. These updates can add, remove, or change edit pairs, affecting which code combinations are allowed.
Organizations that do not monitor updates may experience sudden increases in denials when previously accepted code combinations become invalid.
NCCI and Program Integrity Oversight
NCCI edits are a key program integrity tool. Patterns of repeated NCCI edit overrides—especially without strong documentation—can trigger audits, recoupments, or broader FWA scrutiny.
Because NCCI logic is applied at scale, it is frequently used to identify systemic coding issues rather than isolated errors.
How NCCI (National Correct Coding Initiative) Works in Practice
In practice, NCCI operates as an automated gatekeeper between coding and payment. Most organizations experience NCCI not as a policy document, but as claim denials, edits, or modifier-related rejections that surface only after submission.
Understanding how NCCI functions across the claim lifecycle is key to reducing rework and audit exposure.
Step 1: Services Are Coded Based on Clinical Documentation
NCCI workflows begin with clinical documentation and code selection. Providers assign CPT or HCPCS codes based on what was performed during the encounter.
At this stage, NCCI is not yet visible—but decisions made here (which codes are selected and how documentation is structured) determine whether NCCI edits will later apply.
Step 2: Claims Are Submitted and NCCI Edits Are Applied
When claims are submitted to Medicare (or Medicare Advantage plans that mirror NCCI logic), automated NCCI edits are applied during adjudication.
These edits evaluate whether:
- Two or more billed codes are allowed together
- One service is considered bundled into another
- A modifier is required to indicate distinct services
If an invalid code combination is detected, payment for the Column 2 code is typically denied.
Step 3: Modifiers Are Evaluated for Edit Overrides
For edit pairs that allow overrides, modifiers such as -59 or related modifiers may permit separate payment.
In practice, this means:
- The modifier must be applied correctly
- Documentation must clearly support distinct services
- The services must be separate in time, site, or clinical context
Routine or unsupported modifier use is one of the fastest ways to attract audit attention.
Step 4: Denials, Rework, and Appeals Occur
When NCCI edits are not addressed correctly, claims are denied or partially paid. Billing teams may then:
- Review documentation for modifier support
- Correct and resubmit claims
- Appeal denials when services were distinct but improperly processed
High volumes of NCCI-driven rework often signal upstream coding or documentation issues rather than isolated claim errors.
Step 5: Patterns Are Monitored for Compliance Risk
NCCI is applied at scale, making it an effective tool for identifying patterns. Repeated overrides, high modifier usage, or persistent edit failures can trigger:
- Internal audits
- Payer reviews
- Program integrity investigations tied to FWA
Organizations that proactively monitor NCCI patterns reduce long-term compliance exposure.
NCCI in Billing, Reimbursement, and System Limitations
NCCI directly affects reimbursement accuracy and operational efficiency. While intended to prevent improper billing, it can also create friction when workflows are not aligned.
How NCCI Affects Medicare Billing and Payment
NCCI edits can:
- Deny payment for component services
- Require modifier-supported resubmissions
- Delay cash flow due to rework and appeals
- Reduce reimbursement when errors go uncorrected
Because edits are applied automatically, even small coding inconsistencies can have large financial impact at scale.
NCCI and Modifier-Driven Risk
Modifiers are essential for NCCI compliance—but they are also high-risk. Common issues include:
- Overuse of modifier -59
- Inconsistent modifier application across providers
- Documentation that does not support distinct services
- Reliance on modifiers to “fix” poor coding logic
Auditors often focus on modifier usage patterns when evaluating NCCI compliance.
System Limitations That Drive NCCI Errors
NCCI issues often stem from system and workflow constraints, such as:
- Coding tools that do not surface NCCI edits pre-submission
- Lack of visibility into Column 1 / Column 2 logic
- Inconsistent documentation templates
- Limited education on updated CMS edit tables
- Delayed awareness of quarterly NCCI updates
Organizations with proactive edit monitoring and education programs see fewer denials and lower audit risk.
How NCCI Influences Quality, Access, and Equity in Home Health
While NCCI is a billing control, it indirectly shapes care delivery and patient experience.
NCCI and Quality of Documentation
NCCI incentivizes clearer, more specific documentation. When documentation accurately distinguishes services, billing becomes more defensible and less dependent on corrective modifiers.
However, when documentation is rushed or generic, appropriate services may go unpaid—creating frustration for both providers and patients.
NCCI and Access to Care
Administrative burden tied to NCCI can affect access when providers avoid certain service combinations due to repeated denials or audit concerns.
This can be particularly impactful in settings with complex patients who legitimately require multiple services in a single encounter.
Equity Considerations in NCCI Enforcement
NCCI enforcement can disproportionately affect smaller practices and safety-net providers that lack advanced coding support or analytics tools.
Equity-aware approaches focus on education and workflow improvement rather than punitive enforcement for correctable errors.
Frequently Asked Questions about NCCI
1. What is NCCI (National Correct Coding Initiative)?
NCCI is a set of coding policies and automated edits created by CMS to prevent improper billing of services that should not be reported together under Medicare.
2. What are NCCI edit pairs?
NCCI edit pairs identify CPT or HCPCS code combinations that are not payable together because one service is bundled into another or the services are mutually exclusive.
3. What do Column 1 and Column 2 codes mean in NCCI?
Column 1 codes represent the more comprehensive service, while Column 2 codes represent component services that are generally not paid separately unless an appropriate modifier is used.
4. When can modifiers override NCCI edits?
Some NCCI edits allow modifiers to indicate that services were distinct. Overrides require correct modifier use and documentation that supports separate services.
5. Why do NCCI edits cause so many claim denials?
NCCI edits are applied automatically and at scale. Even small coding inconsistencies or unsupported modifier use can result in denials across many claims.
6. How often does CMS update NCCI edits?
CMS updates NCCI edit tables regularly. Organizations that do not monitor updates may see sudden increases in denials.
7. Can NCCI issues trigger audits or compliance reviews?
Yes. Repeated NCCI overrides or denial patterns can trigger audits, repayment demands, or broader program integrity reviews.
8. Do Medicare Advantage plans use NCCI edits?
Many Medicare Advantage plans follow NCCI logic or use similar edit frameworks, though plan-specific policies may vary.
