What Is FWA (Fraud, Waste, and Abuse) in Healthcare?
Fraud, Waste, and Abuse (FWA) refers to practices that result in improper use of healthcare funds or resources within federally funded programs such as Medicare and Medicaid. While often grouped together, fraud, waste, and abuse represent distinct concepts with different intent, severity, and compliance implications.
From an operational and business standpoint, FWA is a core compliance concern. Healthcare organizations, Medicare Advantage organizations, managed care plans, providers, and vendors are all expected to actively prevent, detect, and report FWA. Failure to do so can result in payment recoupments, penalties, exclusion from federal programs, or enforcement action by oversight bodies such as the Office of Inspector General (OIG).
In practice, FWA is not limited to blatant misconduct. Many FWA findings arise from weak documentation, inconsistent workflows, billing errors, or lack of oversight—making strong operational controls just as important as ethical intent.
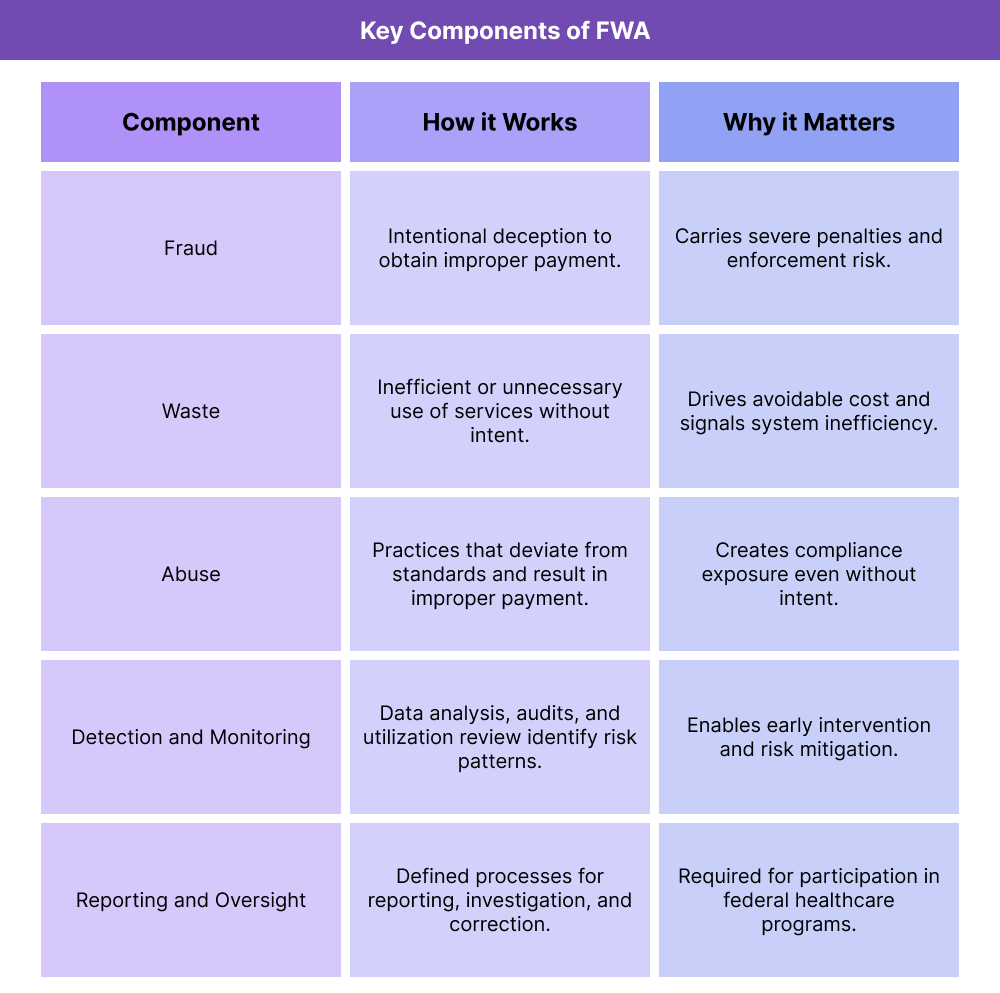
Key Components of Fraud Waste and Abuse (FWA)
Understanding FWA requires distinguishing between its three components and how each shows up in real-world healthcare operations. While the compliance response may overlap, the underlying behaviors and risk profiles differ.
Fraud in Healthcare Programs
Fraud involves intentional deception or misrepresentation to obtain unauthorized payment or benefit. Examples include billing for services not rendered, falsifying records, or knowingly submitting false claims.
From a compliance perspective, fraud carries the highest risk and most severe consequences. Organizations are expected to have controls that prevent intentional misconduct and detect suspicious patterns early.
Waste in Healthcare Operations
Waste refers to the overuse or misuse of services that results in unnecessary cost but does not involve intent to deceive. Common examples include redundant testing, inefficient care delivery, or services that provide little clinical value.
Waste often reflects system design issues rather than individual behavior. Addressing waste typically requires better care coordination, utilization management, and data visibility rather than disciplinary action.
Abuse in Healthcare Billing and Care Delivery
Abuse includes practices that are inconsistent with accepted clinical or billing standards and result in unnecessary cost or improper payment. Unlike fraud, abuse does not require intent, but it still creates compliance risk.
Examples include upcoding, billing for services that are not medically necessary, or failing to meet documentation requirements. Abuse frequently appears in audits when workflows are poorly standardized or staff are inadequately trained.
FWA Detection and Monitoring Mechanisms
Healthcare organizations are expected to actively monitor for FWA using a combination of:
- Claims and encounter data analysis
- Utilization and outlier monitoring
- Documentation reviews
- Referral and prescribing pattern analysis
- Internal audits and compliance reviews
These activities are especially important in Medicare Advantage and managed care environments, where plans are responsible for downstream provider oversight.
Reporting and Oversight Responsibilities
FWA programs include clear expectations for reporting suspected issues. Medicare and Medicaid programs require organizations to:
- Train staff on FWA awareness
- Provide reporting mechanisms (hotlines or escalation paths)
- Investigate credible allegations
- Take corrective action when issues are identified
These responsibilities often intersect with broader compliance programs and OIG guidance.
How FWA (Fraud, Waste, and Abuse) Works in Practice in Healthcare
Fraud, Waste, and Abuse (FWA) becomes operational when healthcare organizations translate high-level compliance expectations into day-to-day workflows. In practice, FWA prevention is less about isolated bad actors and more about whether systems, documentation, and oversight are designed to surface risk early and consistently.
For Medicare Advantage organizations, providers, and vendors, FWA operates as a continuous loop: monitor activity, investigate anomalies, correct issues, and adjust controls.
Step 1: Baseline Compliance Expectations Are Established
FWA prevention starts with clear expectations. Organizations define what compliant behavior looks like across billing, documentation, referrals, prescribing, and care delivery.
This includes:
- Coding and billing standards
- Medical necessity documentation requirements
- Referral and ordering expectations
- Prescribing and pharmacy controls
- Training requirements for staff and downstream partners
These standards are often informed by CMS guidance and OIG enforcement patterns and are embedded into policies, training materials, and system configurations.
Step 2: Activity Is Monitored for FWA Risk Signals
Once services are delivered and claims are submitted, organizations monitor data for patterns that may indicate fraud, waste, or abuse. Common monitoring activities include:
- Claims and encounter outlier analysis
- Utilization trend reviews
- High-risk code and modifier monitoring
- Referral and prescribing pattern analysis
- Comparison of providers against peer benchmarks
In Medicare Advantage, plans are responsible for monitoring downstream providers, making this step especially critical for delegated entities and vendor partners.
Step 3: Potential Issues Are Investigated and Validated
When anomalies are identified, organizations investigate to determine whether the issue reflects fraud, waste, abuse, or a benign operational explanation.
This typically involves:
- Chart and documentation review
- Interviews with clinical or billing staff
- Review of policies and workflows in place at the time
- Assessment of intent, scope, and financial impact
Many findings labeled as “abuse” or “waste” originate here—not from malicious intent, but from unclear guidance, inconsistent documentation, or outdated workflows.
Step 4: Corrective Action and Remediation Occur
Once an issue is confirmed, organizations implement corrective action. Depending on severity, this may include:
- Education or retraining
- Workflow and template updates
- Claims reprocessing or repayment
- Contractual or credentialing changes
- Enhanced monitoring going forward
For Medicare Advantage organizations, corrective action is often documented and tracked to demonstrate compliance during audits or reviews.
Step 5: Oversight, Audits, and Continuous Improvement Continue
FWA prevention is ongoing. Oversight entities—including CMS and OIG—expect organizations to continuously refine controls based on new risks, regulatory changes, and enforcement trends.
This feedback loop drives:
- Updates to compliance programs
- Changes in monitoring logic
- Investment in analytics and care management tools
- Stronger documentation and audit readiness
Organizations that treat FWA as a living operational function—rather than a static policy—are better positioned to reduce risk over time.
FWA in Billing, Reimbursement, and System Limitations
FWA considerations directly affect how healthcare organizations bill, get paid, and manage financial risk. Even small billing inconsistencies can escalate when they occur at scale or intersect with federal funding rules.
How FWA Affects Medicare Billing and Reimbursement
FWA risk often surfaces through billing patterns. In Medicare and Medicare Advantage environments, this can include:
- Services billed without sufficient documentation
- Repeated use of high-risk codes or modifiers
- Billing patterns inconsistent with patient population or diagnosis mix
- Services that appear duplicative or medically unnecessary
When such patterns are identified, organizations may face payment holds, audits, recoupments, or expanded monitoring—even if the underlying care was appropriate.
FWA and Documentation Standards
Documentation is central to distinguishing appropriate care from potential FWA. Weak documentation often turns otherwise acceptable services into compliance risks.
Operationally, this means:
- Clear linkage between diagnosis, service, and medical necessity
- Consistent documentation across providers and settings
- Templates that prompt required elements without encouraging overdocumentation
- Version control so documentation reflects current rules
This is especially important in Medicare Advantage, where encounter data, risk adjustment, and quality reporting intersect with FWA oversight.
System Limitations and Common FWA Risk Drivers
Many FWA findings are driven by system limitations rather than intentional behavior, such as:
- Fragmented systems: billing, clinical, and care management data not aligned
- Poor visibility: limited insight into utilization trends until issues scale
- Inconsistent training: staff applying different standards for similar services
- Delayed feedback: issues identified months after services are delivered
Addressing these gaps often requires better integration, analytics, and workflow standardization—not just more rules.
How FWA Influences Quality, Access, and Equity in Healthcare
FWA programs are designed to protect public funds, but they also shape how care is delivered. How organizations implement FWA controls can either support or undermine broader care goals.
FWA and Healthcare Quality
When well-designed, FWA controls reinforce quality by discouraging unnecessary services and promoting appropriate care. Utilization monitoring can highlight care patterns that warrant review or improvement.
However, overly rigid controls can also discourage appropriate care if providers fear scrutiny. Balancing monitoring with clinical judgment is key to maintaining quality.
FWA and Access to Care
Aggressive FWA enforcement can affect access when providers reduce services, avoid high-risk populations, or limit offerings due to compliance concerns.
Organizations that align FWA monitoring with clear guidance and support can reduce unnecessary barriers while still protecting against improper billing.
Equity Considerations in FWA Programs
Equity challenges can arise when FWA controls disproportionately affect providers serving complex or underserved populations. Higher utilization does not always equal inappropriate care—it may reflect unmet need.
Equity-aware FWA programs:
- Incorporate clinical context into reviews
- Adjust benchmarks for patient complexity
- Provide education before punitive action
- Focus on improvement, not just enforcement
When implemented thoughtfully, FWA programs can protect resources without reinforcing disparities.
Frequently Asked Questions about FWA
1. What is FWA (Fraud, Waste, and Abuse) in healthcare?
FWA stands for Fraud, Waste, and Abuse. It refers to practices that result in improper use of healthcare funds or resources in programs like Medicare and Medicaid. Fraud involves intentional deception, while waste and abuse typically involve unnecessary cost or improper billing without intent to deceive.
2. What is the difference between fraud, waste, and abuse in healthcare?
Fraud is intentional misrepresentation to receive improper payment. Waste is the unnecessary use of services or inefficient practices that increase cost without clinical value. Abuse refers to billing or clinical practices that do not align with accepted standards and result in improper payment, even without intent.
3. How does FWA affect Medicare and Medicare Advantage programs?
FWA programs are a major compliance requirement in Medicare and Medicare Advantage. Plans and providers are expected to monitor billing and care patterns, investigate anomalies, and take corrective action. Persistent issues can lead to audits, payment recoupments, civil penalties, or exclusion risk.
4. What are common examples of healthcare FWA?
Common examples include billing for services not provided, upcoding, duplicate billing, medically unnecessary services, improper referral arrangements, or patterns of prescribing that suggest misuse. Many “abuse” findings stem from weak documentation or inconsistent workflows rather than intentional wrongdoing.
5. How do healthcare organizations detect and prevent FWA?
Organizations prevent FWA through compliance training, monitoring and analytics, internal audits, documentation standards, and clear reporting workflows. Plans often use outlier detection and utilization review, while providers focus on documentation quality and billing accuracy.
6. Why does documentation matter for FWA compliance?
Documentation is often the deciding factor in whether a billed service is defensible. Even appropriate care can become a compliance risk if the record does not support medical necessity, service details, or required billing elements. Strong documentation reduces denials, audits, and recoupment exposure.
7. What should staff do if they suspect fraud, waste, or abuse?
Staff should follow their organization’s reporting process, such as a compliance hotline or escalation pathway, and report concerns promptly. Organizations typically investigate credible allegations, document findings, and take corrective action as needed.
8. How does FWA oversight relate to OIG audits and investigations?
The Office of Inspector General (OIG) plays a major role in enforcing program integrity. OIG findings, audits, and investigations often influence what organizations monitor and how they structure FWA compliance programs.
9. Can FWA controls impact access and equity in healthcare?
Yes. If FWA controls are overly rigid, providers may avoid complex patients or reduce services due to audit concerns. Equity-aware FWA programs incorporate clinical context, recognize patient complexity, and prioritize improvement-focused remediation rather than default punitive action.
