What is API (Application Programming Interface) in Healthcare?
An Application Programming Interface (API) is a set of technical rules and protocols that allows different software systems to communicate and exchange data in a structured way. In healthcare, APIs enable systems such as EHRs, payer platforms, analytics tools, and third-party applications to securely share health information without relying on manual processes or custom integrations.
In practice, healthcare APIs are a core mechanism for interoperability. Rather than moving data through files, faxes, or one-off interfaces, APIs allow systems to request and receive specific data elements on demand. This capability underpins many modern health IT initiatives tied to data access, care coordination, and reporting.
APIs are foundational to current federal interoperability efforts. ONC policy frameworks and CMS programs increasingly assume the use of API-enabled systems to support data exchange, patient access, and integration across healthcare ecosystems.
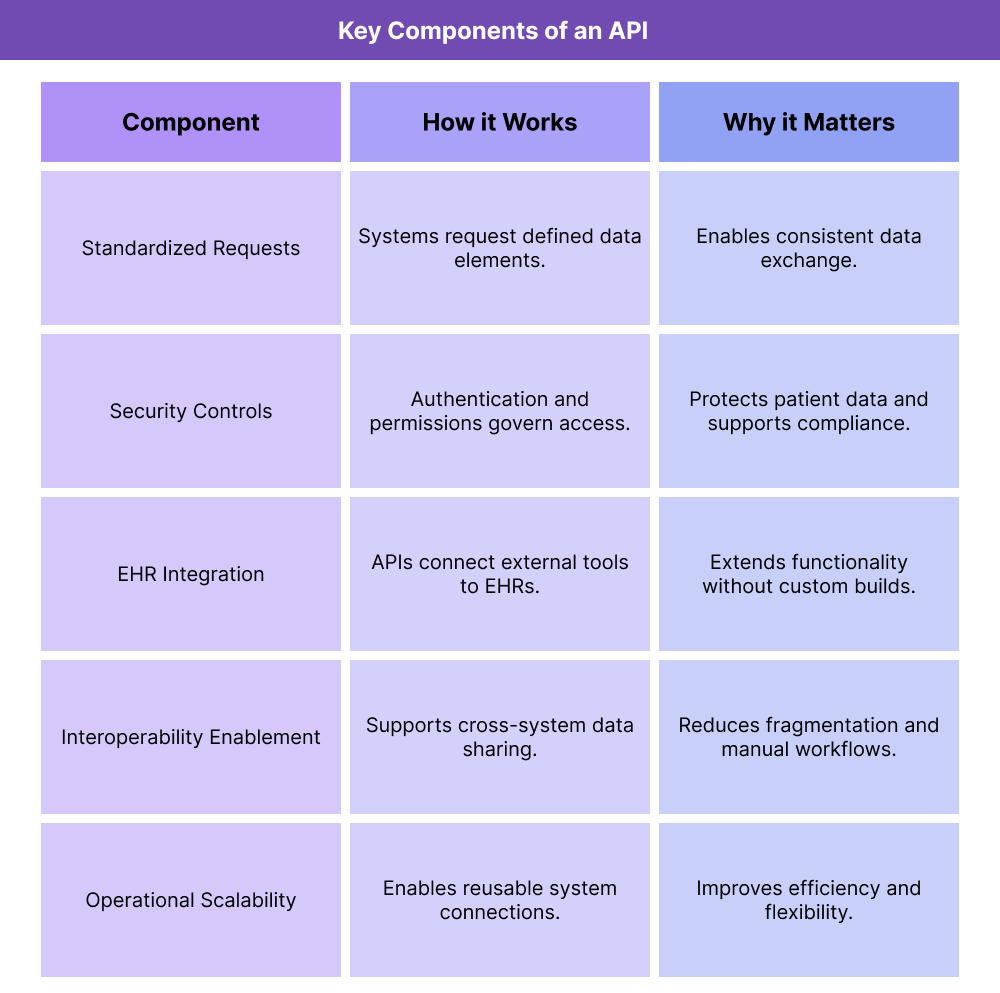
Key Components of an API in Healthcare Systems
Healthcare APIs are not just technical tools; they shape how data moves across organizations and how workflows are designed.
Standardized Data Access and Requests
APIs define how one system can request specific data—such as patient demographics, diagnoses, medications, or encounter history—from another system. Standardized request and response formats reduce ambiguity and improve reliability.
This structured access supports real-time or near-real-time data exchange across systems.
Security, Authentication, and Permissions
Healthcare APIs incorporate security controls to ensure that only authorized users or systems can access sensitive health information. Authentication and permission frameworks determine who can request data and what data they are allowed to receive.
These controls are critical for compliance with privacy and security requirements.
APIs and EHR Integration
EHR APIs allow external applications to interact with core clinical systems without direct database access. This enables functionality such as data ingestion, reporting, analytics, and patient-facing applications.
API-enabled integration reduces the need for custom interfaces and supports scalable system connections.
APIs and Interoperability Initiatives
APIs are a key technical enabler of interoperability policy. Federal initiatives emphasize API-based data exchange to reduce information silos and improve access for providers, patients, and payers.
APIs support use cases such as referrals, care coordination, quality reporting, and patient record access.
Operational Use of APIs in Healthcare
Beyond policy, APIs are used operationally to connect systems across workflows. Common use cases include eligibility checks, clinical data retrieval, analytics integration, and data exchange with third-party platforms.
APIs allow organizations to extend system capabilities without replacing core platforms.
How APIs Work in Practice in Healthcare
In practice, APIs act as the connective tissue between healthcare systems. They allow data to move where it is needed without requiring full system replacement or manual intervention.
Step 1: A System Requests Specific Data
One system sends an API request for defined information—such as a patient record, eligibility status, or clinical data—using standardized parameters.
Step 2: Authentication and Authorization Are Applied
Before data is returned, the receiving system verifies the identity of the requester and checks permissions. Only approved requests are fulfilled.
Step 3: Data Is Returned in a Structured Format
The responding system returns the requested data in a standardized format that the requesting system can process automatically.
Step 4: Data Is Used in Downstream Workflows
Returned data is used to support workflows such as care coordination, reporting, analytics, billing support, or patient access.
Step 5: Ongoing Monitoring and Maintenance
APIs require monitoring to ensure reliability, performance, and security. Changes in standards or system updates may require adjustments over time.
APIs in Billing, Reimbursement, and System Limitations
APIs can automate access to clinical and administrative data needed for billing, coding, and reporting. This improves accuracy and timeliness while reducing rework.
Examples include retrieving diagnosis data, encounter details, or eligibility information.
System Limitations and API Constraints
Despite their benefits, APIs have limitations:
- Not all systems expose the same data
- API access may be limited by vendor policy
- Performance and reliability vary by implementation
- Data may still require normalization or validation
Organizations often need governance and technical oversight to maximize API value.
How APIs Influence Quality, Access, and Equity in Healthcare
APIs affect not only operations, but also care delivery and patient experience.
APIs and Quality of Care
Improved data access enables better-informed clinical decisions, more complete patient records, and stronger coordination across care teams.
APIs and Access to Care
APIs support faster referrals, smoother transitions, and patient access to records. Poorly implemented APIs, however, can create new points of friction.
Equity Considerations in API-Driven Systems
When APIs improve data availability across settings, they can help reduce fragmentation for patients receiving care from multiple providers. Equity challenges arise when access to API-enabled tools is uneven across organizations.
Frequently Asked Questions about APIs in Healthcare
1. What is an API in healthcare?
An API, or Application Programming Interfaces, is a technical interface that allows healthcare software systems to exchange data in a structured and secure way.
2. Why are APIs important for EHR interoperability?
APIs enable EHRs to share data with other systems without custom interfaces, supporting interoperability and data exchange.
3. Are APIs required by healthcare regulations?
Many federal interoperability initiatives assume or require API-based data access, particularly for patient access and data exchange.
4. Do APIs replace traditional interfaces in healthcare?
APIs often reduce reliance on custom interfaces, but many organizations still use a mix of integration methods.
5. How do APIs support patient access to data?
APIs allow applications to retrieve patient data securely, enabling portals, apps, and third-party tools to provide access to records.
6. Can APIs improve billing and reporting accuracy?
Yes. APIs can automate data retrieval for billing and reporting, reducing manual errors and delays.
