HCPCS G0506 Description, Billing Rules, and Use Cases
HCPCS code G0506 is an add-on code used to report a comprehensive assessment and care planning service performed by a physician or other qualified health care professional for patients who require Chronic Care Management (CCM) services. This code captures work that goes beyond the typical monthly CCM activities, including more extensive face-to-face assessment, care coordination, and development of a detailed care plan.
G0506 is billed in addition to a primary monthly care management service and reflects the additional time and complexity involved in evaluating patients with multiple chronic or severe conditions. It is commonly used when a patient’s clinical needs require deeper assessment and planning at the initiation of CCM or during a significant change in clinical status.
What is HCPCS Code G0506?
HCPCS G0506 describes a comprehensive assessment and care planning service performed for patients who are enrolled in or initiating Chronic Care Management. It is reported separately, in addition to the primary monthly CCM service, when the provider performs work that exceeds what is typically included in routine CCM.
Key characteristics of G0506 include:
- A more extensive evaluation of the patient’s chronic conditions
- Development or revision of a comprehensive, patient-centered care plan
- Increased clinical complexity or time beyond standard CCM requirements
- Direct involvement of the billing practitioner
G0506 is intended to recognize the additional clinical effort required to appropriately assess and plan care for patients with complex, multi-condition needs, particularly at the outset of care management or during periods of clinical change.
CMS classifies G0506 as an active physician service code under the Medicare Physician Fee Schedule (MPFS).
HCPCS G0506 Time Thresholds and Code Combinations
HCPCS G0506 is an add-on code and may only be billed when a qualifying primary monthly care management service is also provided. It cannot be billed as a standalone service.
Important to Note:
G0506 requires:
- A patient who qualifies for Chronic Care Management
- Performance of a comprehensive assessment and care planning service
- Work that is over and above standard monthly CCM activities
- Billing by the physician or other qualified health care professional
- Use in addition to a primary CCM code
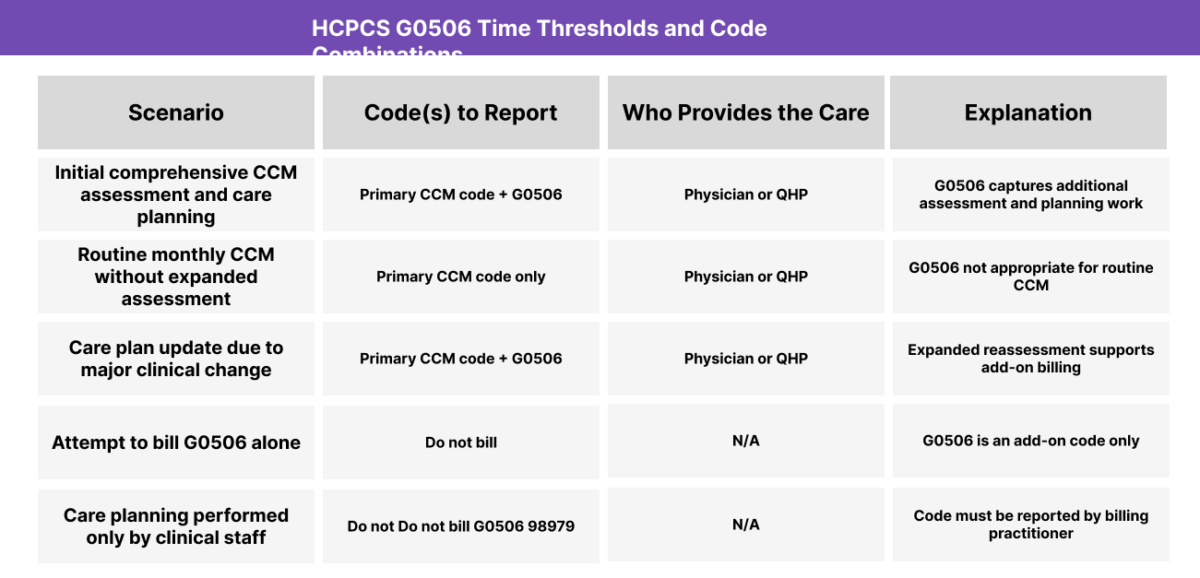
When to Use HCPCS G0506: Common Scenarios and Use Cases
HCPCS G0506 is most often used when a patient’s care requires significantly more assessment and planning than what is typically performed during routine CCM. Here are examples of how HCPCS G0506 is used in practice:
HCPCS G0506 Billing Requirements and Eligibility
HCPCS G0506 may be billed when a patient requires Chronic Care Management and the provider performs additional comprehensive assessment and care planning beyond standard CCM services.
Patient Eligibility Criteria
Patients appropriate for G0506 typically:
- Have multiple chronic or severe conditions
- Require coordinated, longitudinal care management
- Are enrolled in or initiating a CCM program
- Present clinical complexity that necessitates extended assessment and planning
Service Requirements
To qualify for G0506:
- The service must exceed routine CCM assessment and planning
- The work must be performed by the billing practitioner
- A detailed care plan must be developed or significantly revised
- The service must be reported with a primary CCM code
Who Can Bill HCPCS G0506
HCPCS G0506 may be billed only by:
- Physicians
- Other Qualified Health Care Professionals (QHPs)
Note: This code cannot be billed by clinical staff alone and must be reported by the billing practitioner
HCPCS G0506 Billing Documentation Checklist
To support compliant billing of HCPCS G0506, documentation should include:
- Evidence of CCM eligibility
- Multiple chronic conditions requiring ongoing management
- Comprehensive assessment details
- Expanded review of conditions, medications, risks, and care needs
- Care plan documentation
- Clearly documented, patient-centered care plan
- Demonstrates work beyond routine CCM
- Provider involvement
- Documentation showing the service was performed by the billing practitioner
- Primary CCM code linkage
- G0506 billed in addition to a qualifying monthly CCM service
- Attestation that:
- The service exceeded standard CCM requirements
- G0506 was not billed as a standalone service
Common HCPCS G0506 Billing Mistakes (and How to Avoid Them)
❌ Using G0506 for Routine Monthly CCM Work
Routine CCM activities—such as basic care plan updates or standard check-ins—do not justify G0506. Documentation must show additional complexity or depth.
❌ Lack of Comprehensive Assessment Documentation
Claims may be denied if the record does not clearly show a more extensive assessment than what is normally required for CCM.
❌ Clinical Staff Performing the Service Without Provider Involvement
G0506 may only be reported by the billing practitioner. Services performed solely by clinical staff do not qualify.
❌ Failing to Tie the Service to Care Plan Development
The service should clearly result in a detailed care plan or a significant revision. Vague or generic documentation weakens the claim.
❌ Billing G0506 Too Frequently
G0506 is not intended for routine monthly use. It should be reserved for periods when comprehensive assessment and care planning are medically necessary.



