What is PRN (Pro Re Nata) in Healthcare?
PRN (Pro Re Nata) is a clinical abbreviation meaning “as needed.” In healthcare, PRN is used to indicate that a medication, treatment, or intervention should be administered only when specific conditions or symptoms are present, rather than on a fixed schedule.
PRN orders are a common part of clinical care across settings, including acute care, post-acute care, home health, and long-term management. They allow clinicians to provide flexibility in care delivery while still maintaining clinical oversight and intent. PRN use is most often associated with medications, but it can also apply to other treatments or interventions.
From an operational and documentation standpoint, PRN is not simply a convenience term. PRN orders must be clinically justified, clearly defined, and properly documented to support safe care delivery and compliance—particularly in Medicare-regulated programs.
PRN sits at the intersection of Tx (Treatment) decisions, clinical judgment, and documentation accountability. While scheduled treatments are delivered automatically, PRN interventions require active assessment and decision-making at the point of care. This makes PRN a frequent focus in audits and reviews.
Because PRN care is delivered conditionally, ambiguity or poor documentation can create significant risk. Clear PRN usage helps ensure that care remains appropriate, responsive, and defensible throughout the patient’s LOS (Length of Stay).
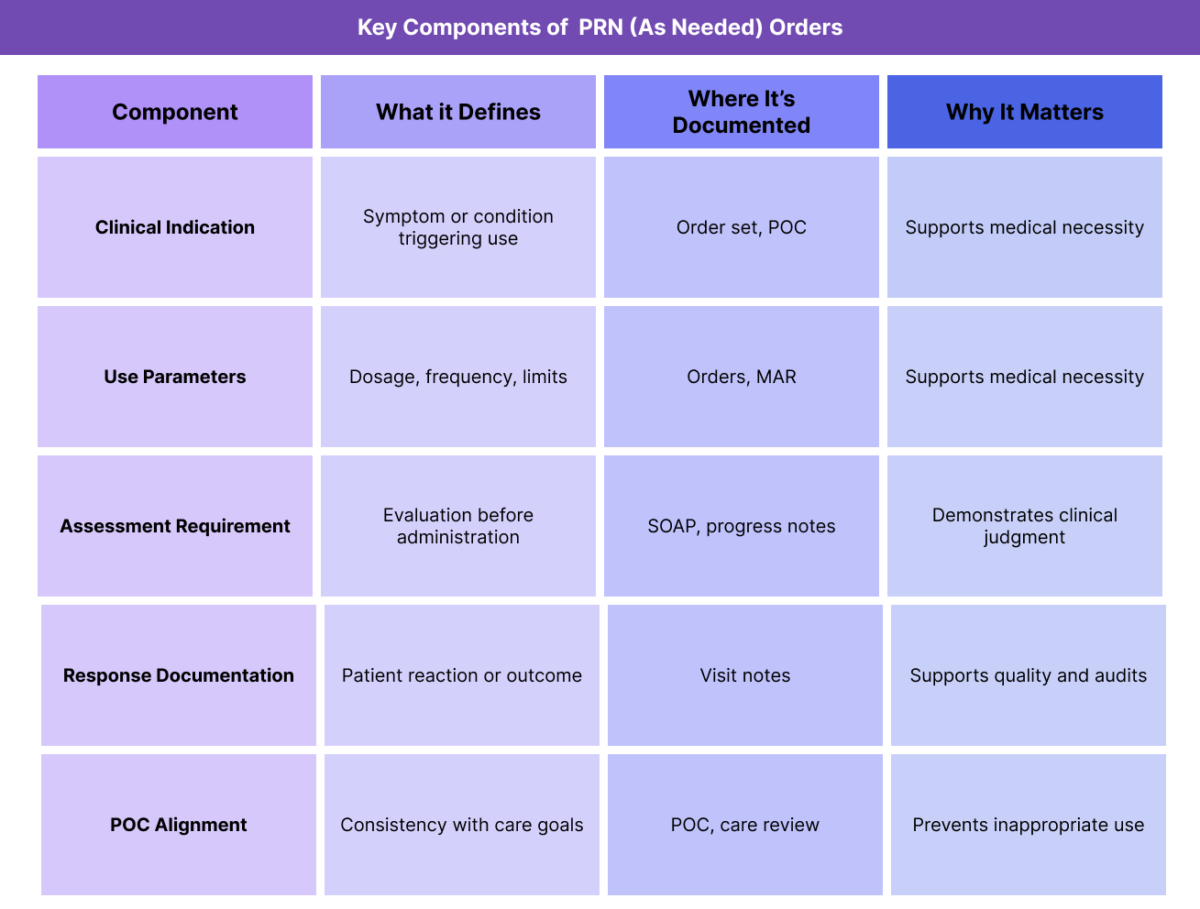
Key Components of PRN Orders and Use
PRN is not a single instruction; it is a structured directive that includes multiple elements which together define when, why, and how an intervention may be provided.
Clear Clinical Indication
Every PRN order must specify why the intervention may be given. This includes the symptom, condition, or clinical trigger that justifies use. Without a clear indication, PRN use becomes subjective and difficult to defend.
A strong PRN order links directly to the patient’s Dx (Diagnosis) or documented symptoms.
Defined Parameters for Use
PRN orders should include boundaries such as frequency limits, dosage limits, or timing restrictions. These parameters protect patient safety and prevent overuse or misuse.
Undefined PRN parameters are a common compliance concern.
Clinical Assessment Before Administration
PRN interventions require assessment at the time of need. Clinicians must determine whether the patient’s current condition meets the criteria outlined in the PRN order.
This assessment is often documented within SOAP notes or the A/P (Assessment and Plan).
Documentation of Administration and Response
When a PRN intervention is provided, documentation should reflect:
- what was given
- why it was given
- how the patient responded
This documentation supports continuity, quality measurement, and reimbursement integrity.
Alignment With the Plan of Care (POC)
PRN use should align with the broader POC (Plan of Care). Frequent PRN use may signal that scheduled treatment adjustments are needed, while lack of PRN use may indicate improvement.
How PRN Works in Practice
PRN interventions are used dynamically throughout an episode of care and require active decision-making.
Initiating PRN Orders at Start of Care (SOC)
PRN orders are often established at SOC (Start of Care) based on the patient’s Dx, symptom history, and anticipated needs. At this stage, clinicians determine which symptoms may require conditional treatment.
Clear PRN definitions at SOC reduce ambiguity later in the episode.
Using PRN During Ongoing Care
Throughout the patient’s LOS (Length of Stay), PRN interventions are used when symptoms arise. Clinicians assess the situation, administer PRN care if appropriate, and document both the rationale and response.
Patterns of PRN use often inform care adjustments.
PRN and Clinical Decision-Making
Frequent PRN use may indicate uncontrolled symptoms or inadequate baseline Tx, prompting reassessment and potential changes to the POC. Conversely, decreasing PRN use may signal improvement.
PRN data provides insight into patient stability and progress.
PRN in Interdisciplinary Care
PRN orders are often reviewed by the IDT (Interdisciplinary Team) to ensure consistency and safety across disciplines. Clear documentation helps prevent duplication or conflicting interventions.
Using PRN Information at Discharge (DC)
At DC (Discharge), PRN usage patterns help inform follow-up recommendations, medication instructions, and patient education. This supports continuity and reduces post-discharge risk.
PRN in Billing, Medical Necessity, and Reimbursement Context
PRN (Pro Re Nata) orders are not billed independently, but they are closely scrutinized in documentation and audit review because they represent conditional care delivery. Unlike scheduled services, PRN interventions require real-time clinical judgment, which makes documentation quality especially important in Medicare-regulated and post-acute care settings.
How PRN Supports Medical Necessity
Medical necessity requires that care be reasonable and necessary at the time it is delivered. PRN interventions must therefore be justified not only by the patient’s Dx (Diagnosis), but also by their current clinical presentation at the moment of use.
Clear PRN documentation helps demonstrate:
- why the intervention was appropriate at that time
- how symptoms aligned with the PRN indication
- that care decisions were clinically justified and patient-specific
When PRN use is documented without clear indication or assessment, reviewers may question whether the intervention was truly necessary.
PRN and Reimbursement Integrity
Although PRN care itself may not be billed separately, PRN documentation often supports the necessity of billed visits, services, or ongoing care. Patterns of PRN use may be evaluated to determine whether:
- visit frequency is justified
- baseline Tx (Treatment) plans are appropriate
- continued services during LOS (Length of Stay) are reasonable
Inconsistent or poorly documented PRN use can weaken the reimbursement narrative, even if overall care delivery was appropriate.
PRN in Episode-Based and Longitudinal Care Models
In episode-based and longitudinal care models, PRN usage provides insight into patient stability, symptom control, and response to care. Reviewers may examine PRN patterns over time to assess whether care decisions evolved appropriately.
High PRN use without plan adjustments can raise concerns, while decreasing PRN use may support discharge readiness.
Common PRN-Related Documentation and Compliance Risks
PRN-related compliance risk is common and often underestimated.
Frequent risk patterns include:
- PRN orders without clear clinical indication
- Missing assessment documentation prior to PRN administration
- PRN interventions documented without patient response
- PRN use not aligned with the POC (Plan of Care)
- Continued PRN use without reassessment or plan updates
Because PRN care is conditional, documentation gaps are more visible during review.
System and Workflow Challenges Affecting PRN Quality
PRN documentation quality is heavily influenced by system design and workflow clarity.
Ambiguous PRN Orders
Orders that simply state “PRN” without defining symptoms, limits, or reassessment criteria create ambiguity. These orders increase both safety and compliance risk.
Fragmented Documentation
When PRN administration, assessment, and response are documented in different places, it becomes difficult to reconstruct clinical reasoning during review.
Limited Decision Support
Without prompts or safeguards, clinicians may administer PRN interventions without fully documenting rationale or outcome, particularly in high-volume settings.
How PRN Influences Quality, Access, and Equity
PRN usage affects patient experience and fairness in care delivery.
PRN and Quality of Care Outcomes
Appropriate PRN use supports symptom control, patient comfort, and responsive care. Poorly managed PRN use can mask underlying issues or delay necessary care plan changes.
PRN and Access to Healthcare Services
PRN interventions can help manage symptoms efficiently, potentially reducing unnecessary visits or escalation. However, inadequate documentation may lead to service limitations or delayed approvals.
Equity Considerations in PRN Use
Patients’ ability to request PRN interventions may be influenced by language barriers, cognitive status, or health literacy. Equity-aware PRN practices ensure that symptom reporting is actively assessed rather than relying solely on patient initiation.
Documenting context and communication supports equitable care delivery.
Frequently Asked Questions about PRN in Healthcare
1. What does PRN mean in healthcare?
PRN stands for Pro Re Nata, meaning “as needed.” It indicates that a medication, treatment, or intervention should be provided only when specific symptoms or conditions are present, rather than on a fixed schedule.
2. How is PRN different from scheduled treatment?
Scheduled treatments are delivered at predetermined intervals, while PRN interventions require real-time assessment and clinical judgment before administration. PRN care is conditional and must be justified at the time of use.
3. Why is PRN documentation important for Medicare compliance?
In Medicare-regulated programs, PRN documentation helps demonstrate that interventions were medically necessary when provided. Poor PRN documentation is a common audit finding.
4. What should be documented when PRN care is provided?
Documentation should include the indication for use, assessment findings, what was administered, and how the patient responded. This supports continuity, safety, and compliance.
5. Can frequent PRN use be a compliance concern?
Yes. Frequent PRN use without reassessment or updates to the care plan can suggest that baseline treatment is insufficient or that care is not being actively managed.
6. How does PRN relate to SOAP and A/P documentation?
PRN assessments and responses are often documented within SOAP notes and reflected in the A/P (Assessment and Plan). Alignment across these sections strengthens documentation quality.
7. Can PRN use affect discharge planning?
Yes. PRN usage patterns may inform discharge readiness and post-discharge planning. Persistent PRN needs may indicate ongoing care requirements.
