What are IADLs (Instrumental Activities of Daily Living in Healthcare?
IADLs (Instrumental Activities of Daily Living) refer to the more complex activities required for an individual to live independently within the community. Unlike ADLs (Activities of Daily Living), which focus on basic self-care, IADLs involve higher-level functional tasks that require cognitive ability, organization, problem-solving, and interaction with the environment.
In healthcare, IADLs are used to assess a patient’s ability to manage daily life beyond basic personal care. These activities often include tasks such as managing medications, preparing meals, handling finances, using transportation, shopping, and maintaining a household. Limitations in IADLs may not prevent a person from performing basic self-care, but they can significantly affect safety, independence, and quality of life.
IADLs are particularly important in post-acute, home health, and longitudinal care settings, where the goal is often to support patients in remaining safely at home. Assessment of IADLs helps clinicians understand whether a patient can function independently or requires additional support services, caregiver involvement, or environmental modifications.
From a care-planning perspective, IADLs bridge the gap between clinical condition and real-world functioning. A patient’s Dx (Diagnosis) and Tx (Treatment) may appear stable, but IADL limitations can reveal ongoing risks that affect LOS (Length of Stay), discharge readiness, and long-term outcomes.
Because IADLs reflect how health conditions impact everyday life, they are a critical component of functional assessment at SOC (Start of Care) and throughout the episode of care.
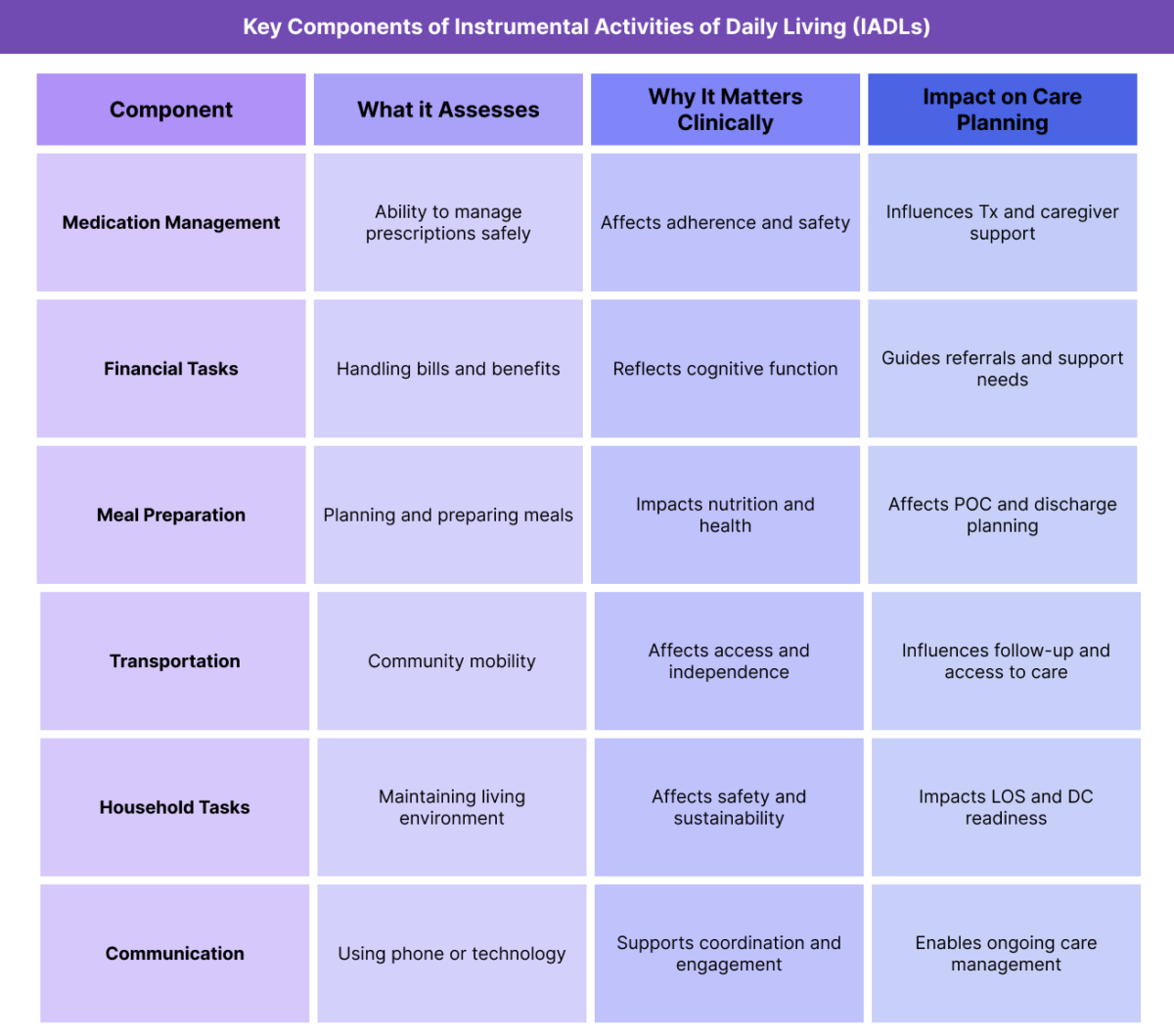
Key Components of Instrumental Activities of Daily Living (IADLs)
IADLs encompass a range of functional domains that together describe a person’s ability to live independently and safely in their environment.
Medication Management
Medication management is one of the most critical IADLs. It includes the ability to understand medication instructions, organize doses, remember schedules, and recognize adverse effects. Impairments in medication management can lead to safety risks, nonadherence, and preventable hospitalizations.
Medication-related IADL limitations often influence care intensity and caregiver involvement.
Financial Management
Financial IADLs involve tasks such as paying bills, budgeting, and managing insurance or benefits. Difficulties in this area may reflect cognitive impairment, executive dysfunction, or social vulnerability.
Financial management challenges are often identified through Hx (History) and may influence discharge planning and referrals.
Meal Preparation and Nutrition
Meal preparation includes planning meals, shopping for groceries, and safely preparing food. Limitations in this area can affect nutrition, medication effectiveness, and overall health.
IADL deficits related to meal preparation may necessitate additional services or education as part of the POC (Plan of Care).
Transportation and Community Mobility
Transportation IADLs assess the patient’s ability to travel safely within the community, whether by driving, using public transportation, or coordinating rides. Transportation limitations can affect access to care, social engagement, and independence.
Household Management
Household IADLs include tasks such as cleaning, laundry, and basic home maintenance. These activities require physical stamina, coordination, and planning.
Household management limitations often contribute to safety concerns and influence discharge readiness.
Communication and Technology Use
Modern IADL assessments increasingly include the ability to use phones, devices, or technology to communicate, manage appointments, or access services. These skills are critical for care coordination in contemporary healthcare settings.
How IADLs Work in Practice
IADLs are assessed and used continuously throughout the care episode to inform clinical and operational decisions.
Assessing IADLs at Start of Care (SOC)
IADL assessment is typically performed at SOC (Start of Care) to establish a functional baseline beyond basic ADLs. Clinicians evaluate which instrumental activities the patient can perform independently and where assistance is required.
This baseline helps contextualize PMH (Past Medical History) and supports accurate care planning.
Using IADLs to Inform Diagnosis and Risk
While IADLs are not diagnoses themselves, limitations may signal cognitive impairment, functional decline, or unmet social needs. These insights can inform Dx refinement and risk stratification.
Guiding Treatment (Tx) and Care Planning
IADL limitations directly influence Tx (Treatment) selection and the structure of the POC. Therapy interventions, education, and caregiver training are often designed to address specific IADL deficits.
Monitoring IADL Changes During LOS
Throughout the patient’s LOS (Length of Stay), clinicians reassess IADLs to track improvement or decline. Changes in IADL performance often guide decisions about care continuation or modification.
Using IADLs to Determine Discharge Readiness (DC)
At DC (Discharge), IADL performance is a key indicator of whether a patient can safely live independently or requires ongoing support. IADL findings help shape discharge recommendations and follow-up planning.
IADLs in Billing, Medical Necessity, and Reimbursement Context
IADLs (Instrumental Activities of Daily Living) are not billed as standalone services, but they play a significant supporting role in how medical necessity, care intensity, and service duration are evaluated—particularly in Medicare-regulated and post-acute care settings.
How IADLs Support Medical Necessity
Medical necessity is assessed based on how a patient’s condition affects their ability to function safely and independently. IADL limitations help explain why skilled services are required even when a patient can perform basic ADLs (Activities of Daily Living).
For example, a patient who can bathe and dress independently but cannot manage medications or transportation may still require skilled care. IADL deficits provide the functional justification for:
- therapy services
- care coordination
- caregiver education
- extended LOS (Length of Stay)
Clear IADL documentation strengthens the rationale for ongoing Tx (Treatment) and supports alignment with the POC (Plan of Care).
IADLs and Reimbursement Integrity
Accurate IADL documentation helps ensure reimbursement reflects patient complexity. Functional limitations related to cognition, organization, or community mobility often explain why care requires more time, resources, or interdisciplinary involvement.
When IADL limitations are understated or omitted, care may appear excessive during review. Conversely, unsupported IADL deficits increase audit risk.
IADLs in Episode-Based and Longitudinal Care Models
In episode-based and longitudinal care models, IADLs are used to evaluate whether care progression aligns with functional improvement. Reviewers may assess whether:
- IADL limitations improved during the episode
- care decisions were adjusted based on functional change
- discharge timing was appropriate given IADL status
Strong IADL tracking supports defensible care decisions from SOC (Start of Care) through DC (Discharge).
Common IADL-Related Documentation and Compliance Risks
IADL-related compliance issues often stem from documentation inconsistency rather than inappropriate care.
Common risks include:
- IADL deficits documented at SOC but not revisited
- Inconsistent IADL findings across disciplines
- IADL limitations not aligned with Dx or Tx
- Functional deficits described without clear examples
- Copy-forward IADL documentation without reassessment
Auditors may question care necessity when IADL documentation lacks specificity or continuity.
System and Workflow Challenges Affecting IADL Documentation
Accurate IADL assessment and documentation depend heavily on workflow design and system support.
Fragmented Functional Assessments
When IADL information is captured in multiple locations or formats, clinicians may lack a unified view of patient function. Fragmentation increases the risk of conflicting documentation.
Limited Reassessment During LOS
IADLs are sometimes assessed only at SOC and DC. Without interim reassessment, documentation may fail to reflect meaningful progress or decline.
Inconsistent IDT Visibility
If IADL information is not easily accessible to the IDT (Interdisciplinary Team), care planning and coordination may suffer. Shared visibility supports aligned decision-making.
How IADLs Influence Quality, Access, and Equity
IADLs directly affect patient outcomes and fairness in care delivery.
IADLs and Quality of Care Outcomes
Improvement in IADLs is often a primary goal of post-acute and home-based care. Accurate assessment helps clinicians tailor Tx, monitor progress, and identify when additional support is needed.
Poor IADL documentation can obscure risk and delay appropriate interventions.
IADLs and Access to Healthcare Services
IADL limitations frequently influence eligibility for services, discharge planning, and follow-up care. Clear documentation supports timely access to appropriate care and resources.
Equity Considerations in IADL Assessment
Socioeconomic factors, cultural norms, and access to resources can affect IADL performance. For example, transportation or financial management limitations may reflect systemic barriers rather than individual capability.
Equity-aware IADL assessment distinguishes between functional impairment and environmental constraints, supporting fairer care decisions.
Frequently Asked Questions about IADLs in Healthcare
1. What does IADL mean in healthcare?
IADL stands for Instrumental Activities of Daily Living and refers to complex tasks required for independent living, such as managing medications, finances, transportation, and household responsibilities.
2. How are IADLs different from ADLs?
ADLs focus on basic self-care tasks like bathing and dressing, while IADLs involve higher-level activities that require cognitive and organizational skills. Both are used together to assess functional status.
3. Why are IADLs important in post-acute care?
IADLs help determine whether a patient can live safely at home and manage daily life. Limitations often justify skilled services, caregiver support, or extended care.
4. How are IADLs assessed?
IADLs are assessed through patient interviews, observation, standardized tools, and caregiver input. Assessment typically occurs at SOC and is revisited throughout LOS.
5. Can IADL limitations change during care?
Yes. IADL performance may improve or decline over time. Changes should be documented to support ongoing care decisions and discharge planning.
6. How do IADLs affect discharge decisions?
At DC, IADL status helps determine whether a patient can safely live independently or requires ongoing support. IADL findings often guide referrals and follow-up planning.
7. Can poor IADL documentation affect audits or payment?
Yes. Incomplete or inconsistent IADL documentation can weaken medical necessity justification and increase audit risk, even when care was appropriate.
