What is CDS (Clinical Decision Support) in Healthcare?
Clinical Decision Support (CDS) refers to tools and functionalities within health information systems that provide clinicians with patient-specific guidance, alerts, or recommendations to support clinical decision-making. CDS is designed to improve care quality, safety, and consistency by delivering relevant information at the point of care.
In practice, CDS operates within or alongside EHR systems, using structured clinical data—such as diagnoses, medications, lab results, and care plans—to surface reminders, warnings, or evidence-based recommendations. CDS does not replace clinical judgment; instead, it supports clinicians by highlighting risks, gaps, or best practices in real time.
CDS plays an increasingly important role in Medicare-regulated environments, where quality measurement, guideline adherence, and documentation consistency directly affect reimbursement, audit risk, and performance outcomes.
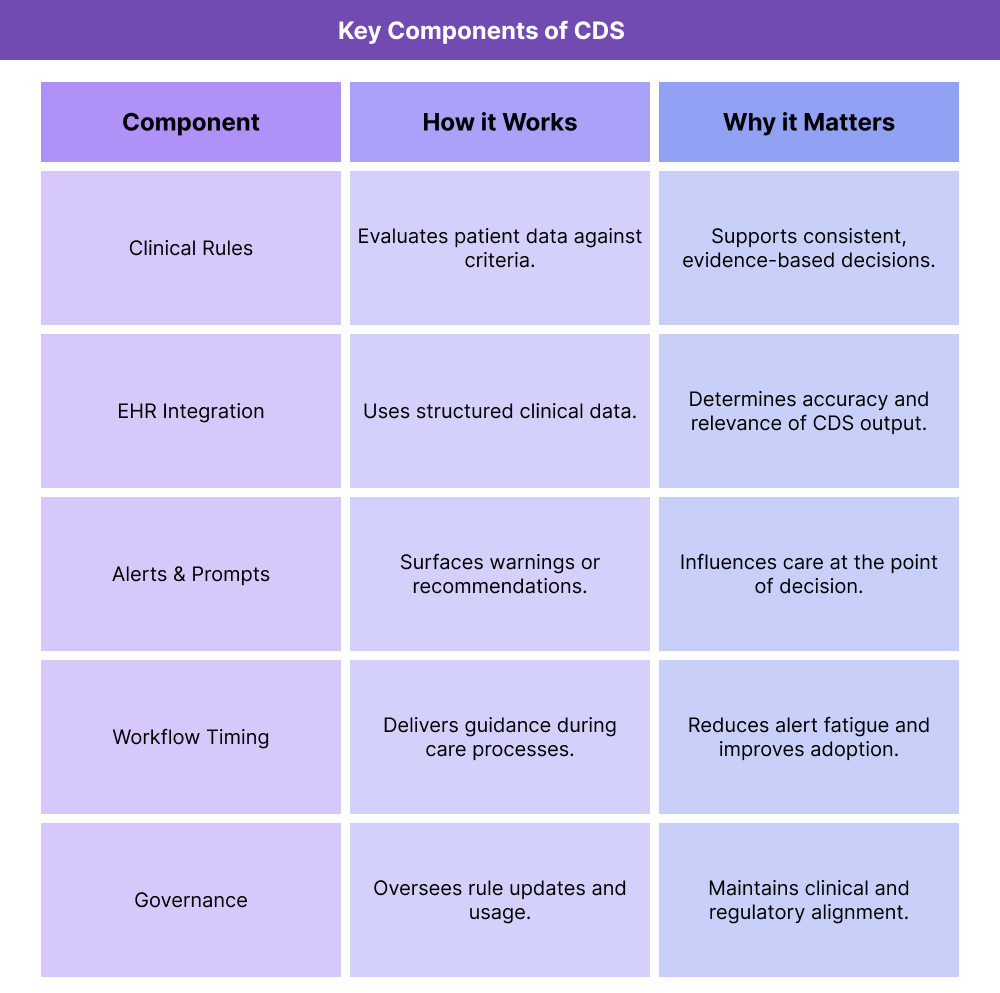
Key Components of an CDS in Healthcare Systems
CDS systems vary widely in complexity, but effective CDS tools share common structural and operational elements.
Clinical Rules and Logic
At the core of CDS are rules or algorithms that evaluate patient data against defined criteria. These rules may be based on clinical guidelines, safety thresholds, or organizational policies.
Examples include drug–drug interaction checks, preventive care reminders, or alerts for missing documentation.
Integration With EHR Data
CDS relies on structured EHR data to function accurately. Diagnoses, medications, lab values, and encounter details must be captured consistently for CDS tools to trigger appropriately.
Poor data quality or inconsistent documentation can significantly reduce CDS effectiveness.
Alerts, Reminders, and Recommendations
CDS outputs often take the form of alerts, prompts, or suggested actions presented to clinicians during workflows. These may include warnings, reminders, or evidence-based recommendations.
Well-designed CDS balances usefulness with usability to avoid alert fatigue.
Timing and Workflow Placement
Effective CDS delivers information at the right time and place within the clinical workflow. Poorly timed alerts are often ignored, while well-integrated CDS can meaningfully influence decisions.
Workflow alignment is critical for adoption and impact.
Governance and Ongoing Maintenance
CDS tools require governance to ensure rules remain current, clinically appropriate, and aligned with organizational goals. Regular review and updates are necessary as guidelines, policies, and regulations evolve.
How CDS Works in Practice
In practice, CDS functions as a layer of intelligence on top of clinical data, translating information into actionable insights during care delivery.
Step 1: Patient Data Is Captured in the EHR
CDS begins with structured clinical documentation. Diagnoses, medications, lab results, and care plans entered into the EHR provide the data foundation for decision support.
Step 2: CDS Logic Evaluates the Data
CDS rules analyze patient data in real time or near real time, comparing it against defined thresholds, guidelines, or risk indicators.
Step 3: Guidance Is Presented to the Clinician
When criteria are met, CDS tools present alerts, reminders, or recommendations within the clinical workflow. These prompts support safer, more consistent decisions.
Step 4: Clinician Action and Documentation
Clinicians may act on CDS guidance, override it, or document rationale for alternative decisions. Documentation of responses can be important for quality and audit purposes.
Step 5: Monitoring and Optimization
Organizations monitor CDS performance to assess effectiveness, alert burden, and outcomes. Adjustments are made to improve relevance and reduce noise.
CDS in Billing, Reimbursement, and System Limitations
Although CDS does not bill directly, it strongly influences documentation quality and compliance outcomes.
How CDS Supports Billing and Documentation
By prompting clinicians to address care gaps or document required elements, CDS can improve documentation completeness. Strong documentation supports medical necessity, coding accuracy, and audit defensibility.
CDS and Compliance Risk
Poorly designed CDS can create risk if alerts are ignored, overridden without documentation, or misaligned with billing rules. Governance is essential to ensure CDS supports—not undermines—compliance.
System Limitations and CDS Challenges
Common CDS limitations include:
- Alert fatigue reducing effectiveness
- Dependence on data quality
- Difficulty aligning CDS with evolving guidelines
- Variability in vendor implementation
These challenges require ongoing management rather than one-time deployment.
How CDS Influences Quality, Access, and Equity in Healthcare
CDS affects not only clinical decisions, but broader care outcomes.
CDS and Quality of Care
CDS supports quality improvement by reinforcing evidence-based practices, reducing variation, and identifying risks early. When aligned with quality programs, CDS can help close care gaps.
CDS and Access to Care
By supporting efficient decision-making and care prioritization, CDS can improve throughput and reduce delays. Poorly designed CDS, however, can slow workflows.
Equity Considerations in CDS Use
Equity risks arise when CDS logic is based on incomplete or biased data. Equity-aware CDS design considers diverse populations, social context, and transparency in decision logic.
Frequently Asked Questions about CDS (Clinical Decision Support)
1. What is CDS in healthcare?
CDS (Clinical Decision Support) refers to tools that provide clinicians with patient-specific guidance, alerts, or recommendations to support clinical decision-making.
2. Is CDS the same as an EHR?
No. CDS operates within or alongside EHRs, using EHR data to provide guidance, but it is not the EHR itself.
3. How does CDS improve quality of care?
CDS reinforces evidence-based practices, identifies risks, and helps clinicians address care gaps consistently.
4. Can CDS affect billing and compliance?
Yes. CDS can improve documentation quality, but poorly governed CDS can increase compliance risk.
5. What is alert fatigue in CDS?
Alert fatigue occurs when clinicians receive too many or poorly timed alerts, reducing attention to important guidance.
6. Does Medicare require CDS?
Medicare does not mandate specific CDS tools, but many quality and safety expectations assume effective decision support.
7. How is CDS governed in healthcare organizations?
CDS governance involves reviewing rules, monitoring performance, and updating logic to align with clinical guidelines and regulations.
