What is CAD (Coronary Artery Disease) in Healthcare?
CAD (Coronary Artery Disease) is a chronic cardiovascular condition caused by atherosclerotic plaque buildup in the coronary arteries, resulting in reduced blood flow to the heart muscle. In healthcare documentation and provider workflows, CAD is treated as a chronic manifestation of ASCVD, not an episodic diagnosis tied to a single cardiac event.
From a B2B and operational standpoint, CAD is one of the most commonly documented cardiovascular conditions in adult and Medicare populations. It frequently appears on problem lists, risk assessments, and longitudinal care plans, particularly in patients with HTN, ASCVD, CKD, PAD, CHF, or AFib.
CAD is especially relevant in chronic care contexts because it represents ongoing ischemic risk, even when patients are clinically stable or asymptomatic. Providers document CAD to explain why sustained monitoring, medication management, and reassessment are appropriate across time and care settings.
Unlike acute coronary syndromes, CAD is inherently longitudinal. Documentation focuses on disease presence, progression risk, and interaction with comorbid conditions, supporting consistent care planning across a patient’s LOS (Length of Stay) and transitions of care.
Operationally, CAD often functions as a cardiovascular risk anchor, helping explain why patients require ongoing oversight and conservative management even outside of acute events.
Key Clinical and Operational Components of CAD in Healthcare
CAD’s significance lies in how it contributes to long-term ischemic risk, interacts with other chronic conditions, and shapes longitudinal documentation strategy.
CAD as a Manifestation of ASCVD
CAD is widely recognized as a coronary manifestation of atherosclerotic cardiovascular disease (ASCVD). Providers document CAD to indicate that atherosclerosis is present in the coronary circulation, elevating risk for ischemic complications.
This framing supports a unified cardiovascular risk narrative.
CAD and Longitudinal Ischemic Risk
CAD is documented to establish ongoing risk for myocardial ischemia and related complications. Even when symptoms are controlled or absent, CAD signals persistent risk that informs monitoring and management decisions.
Risk context remains relevant throughout long-term care.
CAD in Diagnosis and Problem List Management
CAD typically appears on the problem list as an active chronic condition. Consistent CAD documentation supports clarity across progress notes, care plans, and transitions of care.
Clear problem list management reduces ambiguity when multiple providers are involved.
CAD and Comorbidity Interaction
CAD frequently coexists with HTN, CKD, PAD, CHF, and AFib. Providers document CAD to explain how coronary disease compounds overall cardiovascular risk and increases care complexity.
This interaction supports more comprehensive, defensible risk documentation.
CAD and Long-Term Treatment Strategy
CAD management emphasizes long-term Tx (Treatment) and risk reduction rather than episodic intervention. Providers document CAD to justify sustained management strategies, medication oversight, and longitudinal reassessment.
This reinforces CAD’s role as a chronic care condition.
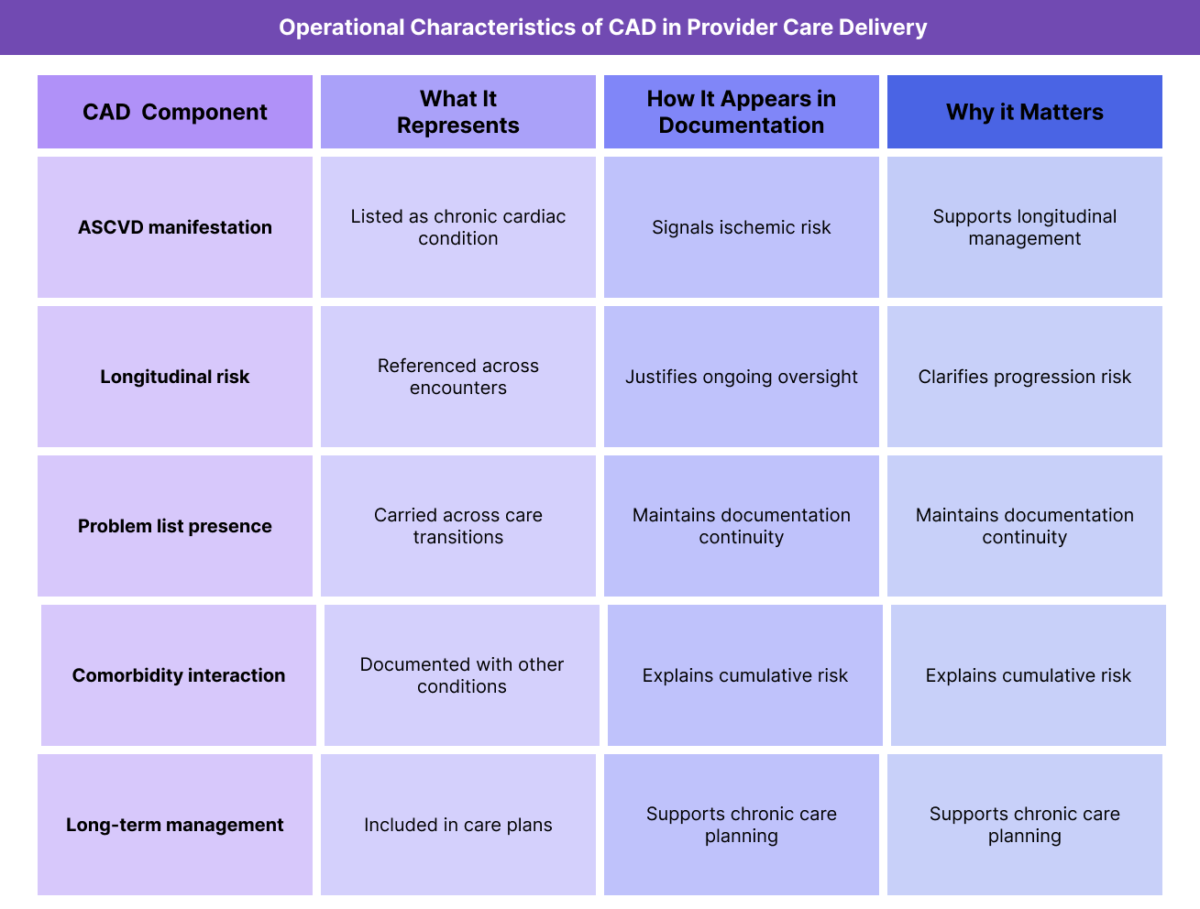
How CAD Is Managed in Practice
CAD management is documentation-driven and longitudinal, particularly in chronic and Medicare-focused care settings.
CAD at Start of Care (SOC)
At SOC (Start of Care), CAD may be documented based on medical history, referral records, or prior cardiac diagnoses. This establishes CAD as part of the patient’s chronic cardiovascular risk profile and frames baseline management considerations.
Documenting source and context improves clarity.
CAD During Ongoing Care and LOS
Throughout a patient’s LOS, CAD status is referenced to contextualize monitoring decisions, medication management, and reassessment needs. Even when stable, CAD remains relevant to care planning.
Consistency across encounters supports longitudinal narratives.
CAD and Interdisciplinary Communication
CAD is a universally recognized condition across disciplines. Clear documentation helps the IDT maintain shared understanding of coronary risk and long-term management priorities.
This is especially important during transitions of care.
CAD as Context for Care Planning
CAD is often documented to explain why patients require sustained monitoring, risk management, and coordination despite limited acute symptoms. It provides coronary-specific risk context that complements broader ASCVD documentation.
CAD in Billing, Reimbursement, and System Limitations
How CAD Supports Medical Necessity Documentation
CAD (Coronary Artery Disease) is not a billable service on its own, but it provides essential clinical risk context that supports medical necessity for ongoing monitoring, management, and coordination of care. In Medicare and other payer environments, CAD documentation helps establish persistent ischemic risk that justifies longitudinal oversight rather than episodic care.
By documenting CAD as an active condition, providers signal that coronary disease continues to influence clinical decision-making even when patients are clinically stable.
CAD and Justification of Longitudinal Care
CAD is frequently used to justify care delivered over time, particularly when patients are not experiencing acute coronary events. Its chronic nature explains why continued follow-up, medication management, and reassessment remain appropriate across encounters.
In reimbursement review, CAD often contextualizes:
- duration of care
- follow-up cadence
- ongoing inclusion in care plans
- coordination across providers and settings
This is especially relevant when CAD coexists with HTN, ASCVD, CKD, PAD, CHF, or AFib.
CAD as Supporting Context, Not a Billing Trigger
CAD should not be positioned as the reason a service is billed. Instead, it functions as supporting documentation that helps reviewers understand why care decisions are reasonable given the patient’s coronary disease burden.
CAD adds the most value when it is integrated into the broader clinical narrative and linked to monitoring, medication oversight, or risk-management decisions.
Reimbursement Risk When CAD Is Poorly Documented
CAD documentation can weaken reimbursement support when it is:
- listed without explanation of current relevance
- inconsistently documented across encounters
- copied forward without acknowledgment of stability or progression
- disconnected from care planning or monitoring decisions
Clear, intentional CAD documentation reduces ambiguity and strengthens defensibility during payer review.
How CAD Influences Quality, Access, and Equity in Healthcare
CAD and Quality-Aligned Care Documentation
From a quality perspective, CAD documentation supports consistency and continuity, not direct intervention. Accurate CAD documentation ensures providers maintain a shared understanding of coronary disease burden and align care decisions accordingly.
Quality-aligned documentation reflects that CAD risk is actively considered in longitudinal planning rather than treated as historical background.
CAD and Care Coordination Across Settings
CAD commonly follows patients across primary care, specialty care, post-acute environments, and home-based services. Consistent documentation helps ensure coronary risk is recognized during transitions of care and appropriately factored into ongoing management.
Clear CAD documentation reduces fragmentation when multiple providers contribute to the record.
CAD and Access to Appropriate Services
CAD documentation can influence access to services by clarifying ischemic risk that may not be evident from acute findings alone. Clear documentation supports appropriate follow-up planning, monitoring intensity, and coordination decisions.
This helps prevent both under-recognition of disease burden and unnecessary escalation.
Equity Considerations in CAD Documentation
CAD prevalence, diagnosis, and management are influenced by social determinants of health, including access to preventive care, diagnostic testing, medications, and specialty follow-up. Equity-aware CAD documentation acknowledges these factors when relevant.
Documenting barriers to consistent care or delayed diagnosis helps ensure CAD assessment reflects patient reality rather than system access alone.
Avoiding Bias in CAD Interpretation
Providers should avoid assumptions about disease severity or engagement based solely on demographic factors. CAD risk and progression are shaped by access, comorbidities, and systemic barriers.
Thoughtful documentation supports fair, individualized assessment of coronary disease burden.
Frequently Asked Questions about CAD
1. What is CAD in healthcare?
CAD (Coronary Artery Disease) is a chronic cardiovascular condition caused by atherosclerotic plaque buildup in the coronary arteries, leading to reduced blood flow to the heart muscle. In healthcare documentation, CAD is used to describe ongoing ischemic risk rather than a single acute cardiac event.
2. Is CAD considered a chronic condition?
Yes. CAD is documented as a chronic condition because coronary atherosclerosis represents persistent disease that carries ongoing risk for progression and complications over time.
3. Does CAD affect billing or reimbursement directly?
CAD is not billable on its own. However, it supports reimbursement documentation by providing clinical context that explains why longitudinal monitoring, medication management, and coordinated care are appropriate.
4. How is CAD used in medical necessity review?
CAD supports medical necessity by establishing persistent coronary disease burden and ischemic risk. This helps explain why care continues over time even when patients are not experiencing acute symptoms.
5. How does CAD differ from ASCVD?
ASCVD is a broad classification describing atherosclerotic cardiovascular disease across the body, while CAD refers specifically to atherosclerotic disease affecting the coronary arteries. CAD is commonly documented as a manifestation of ASCVD.
6. What are common CAD documentation issues?
Common issues include inconsistent problem list usage, lack of clarity around current relevance, and failure to integrate CAD into longitudinal care planning.
7. Why do reviewers pay attention to CAD documentation?
Reviewers evaluate whether documentation clearly explains coronary disease burden and supports care decisions. CAD is a widely recognized indicator of long-term ischemic risk when documented consistently.
