CPT 98979 Description, Billing Rules, & Use Cases
CPT 98979 is used to report Remote Therapeutic Monitoring (RTM) treatment management services when a physician or other qualified health care professional provides at least 10 minutes of RTM management time in a calendar month and completes at least one real-time, interactive communication with the patient or caregiver. RTM treatment management involves the clinical work required to review therapy-related data, assess patient response or adherence, communicate with the patient, and make informed decisions about ongoing therapy or intervention.
Unlike RTM device supply codes, CPT 98979 reflects active clinical management, not the technology itself. It is commonly used alongside RTM device supply codes (such as those supporting respiratory or musculoskeletal monitoring) when therapeutic data is being collected and used to guide care outside of traditional in-office visits.
CPT 98979 represents the first 10 minutes of RTM treatment management time in the month. Additional time beyond this initial threshold is reported separately using add-on RTM management codes when applicable.
What is CPT Code 98979?
CPT 98979 covers physician or other qualified health care professional time spent managing a patient enrolled in a Remote Therapeutic Monitoring program. It is billed once per calendar month when all of the following criteria are met:
- The patient is actively enrolled in an RTM program
- Therapeutic monitoring data (e.g., adherence, response, intervention metrics) is available for review
- The provider performs at least 10 minutes of cumulative RTM treatment management work during the month
- The month includes at least one real-time, interactive communication with the patient or caregiver
CPT 98979 does not include:
- RTM device supply or data access/transmission (reported separately under RTM device supply codes)
- RTM setup or onboarding services
- Non-clinical or administrative tasks
Instead, CPT 98979 captures the clinical decision-making and patient-facing work associated with RTM, such as reviewing therapy data, identifying issues or trends, contacting the patient, adjusting therapy plans, and documenting follow-up actions.
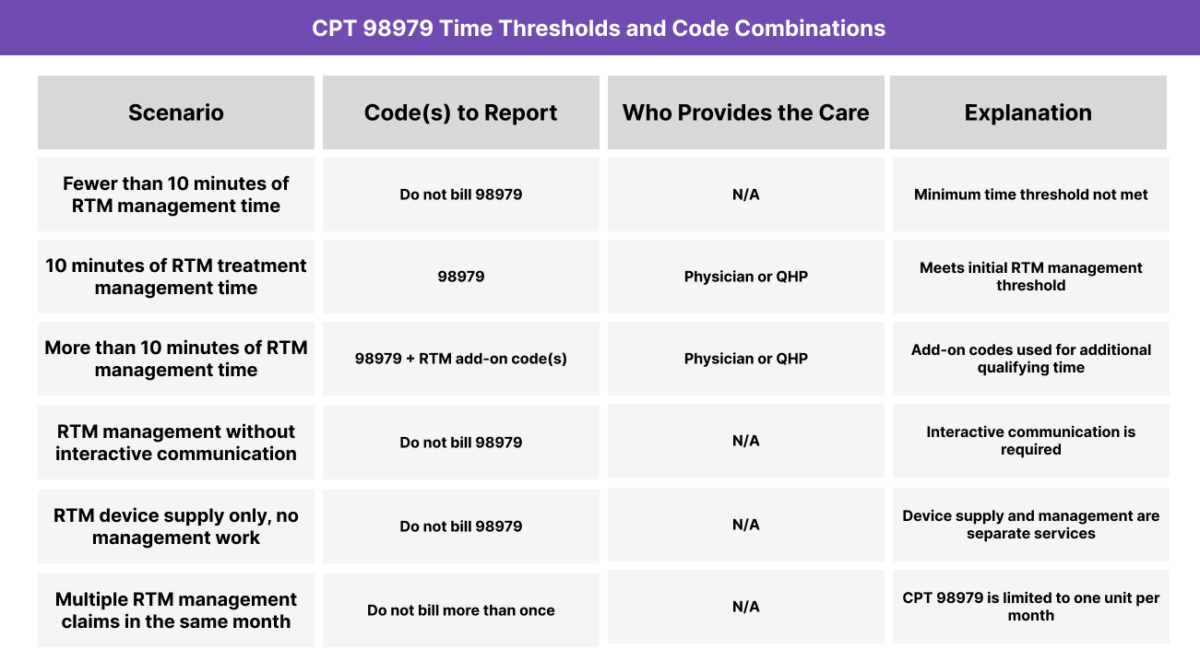
CPT 98979 Time Thresholds and Code Combinations
CPT 98979 may be billed once per calendar month to report the first 10 minutes of RTM treatment management time. Accurate time tracking and documentation are essential, as RTM management codes are cumulative and threshold-based.
Important to Note:
CPT 98979 requires:
- At least 10 minutes of cumulative RTM treatment management time in the month
- One or more real-time, interactive communications with the patient or caregiver
- Time spent by a physician or other qualified health care professional
- One billing instance per patient per calendar month
When to Use CPT 98979: Common Scenarios and Use Cases
CPT 98979 is used when therapeutic monitoring data is actively reviewed and acted upon, but total RTM management time in the month is limited to the initial threshold. Here are examples of how CPT 98979 is used in practice:
CPT 98979 Billing Requirements and Eligibility
CPT 98979 is used to report RTM treatment management services when a physician or qualified health care professional spends at least 10 minutes managing therapeutic monitoring data in a calendar month and completes at least one interactive communication.
Patient Eligibility Criteria
Patients eligible for RTM treatment management typically:
- Are enrolled in an active RTM program
- Are using an RTM device or digital therapeutic tool that generates therapy-related data
- Have a condition or therapy plan that requires provider oversight and intervention
RTM treatment management may be appropriate for:
- Therapy adherence monitoring
- Therapy response evaluation
- Digital therapeutic interventions
- Short-term or episodic therapy oversight
Service Requirements
To qualify for CPT 98979:
- RTM data must be reviewed and inform clinical decision-making
- Total cumulative time must reach at least 10 minutes in the calendar month
- At least one real-time, interactive communication must occur
Time must reflect clinical work such as:
- Reviewing therapy adherence or response data
- Assessing risks or progress
- Communicating recommendations to the patient or caregiver
- Adjusting therapy plans or next steps
- Documenting actions taken
Who Can Bill CPT 98979
CPT 98979 may be billed by:
CPT 98985 Billing Documentation Checklist
- RTM order and monitoring plan
- Clinical rationale for therapeutic monitoring
- Description of therapy or intervention being monitored
- Evidence of RTM data availability
- Therapy-related data available during the billing month
- Monthly time documentation
- At least 10 minutes of cumulative RTM management time
- Description of work performed (not just time totals)
- Interactive communication record
- Date and type of real-time communication
- Summary of discussion and outcomes
- Clinical actions and follow-up
- Therapy adjustments, education, or escalation
- Notes linking actions to RTM data
- Provider identification
- Claim billed under a physician or QHP
- Attestation that:
- Only one unit of CPT 98979 was billed for the month
- RTM management was not duplicated by another provider
Common CPT 98979 Billing Mistakes (and How to Avoid Them)
❌ Billing CPT 98979 With Fewer Than 10 Minutes of Total Time
CPT 98979 requires a minimum of 10 minutes of cumulative RTM treatment management time in the calendar month. If documented time falls below this threshold, the service does not qualify. Tracking time consistently throughout the month helps avoid end-of-cycle billing errors.
❌ No Real-Time Interactive Communication Documented
At least one real-time, interactive communication with the patient or caregiver is required. Asynchronous messages alone typically do not qualify. Documentation should clearly reflect when the interaction occurred and what clinical issues were addressed.
❌ Incorrect Use of RTM Add-On Codes
CPT 98979 captures only the first 10 minutes of RTM management time. Additional time must be supported by documentation and reported using the appropriate add-on code. Billing add-on time without meeting base requirements can trigger denials.
❌ Counting Administrative or Non-Clinical Time
Only time spent on qualifying RTM treatment management activities should be counted. Administrative work, scheduling, or technical troubleshooting unrelated to clinical decision-making should be excluded.
❌ Time Logged Without Clinical Context
Time totals alone are insufficient. Documentation should describe what RTM data was reviewed, what issue or trend was identified, and what action was taken as a result.
❌ Billing Without Clear RTM Enrollment or Data
If the record does not clearly show that the patient was enrolled in RTM and that therapy-related data was available and reviewed, payers may question medical necessity or whether the service occurred.


