CPT 99470 Description, Billing Rules, & Use Cases
CPT 99470 is used to report Remote Physiologic Monitoring (RPM) treatment management services when clinical staff, a physician, or other qualified healthcare professional provides at least 10 minutes but fewer than 20 minutes of RPM management time in a calendar month. This code supports RPM programs where patient-generated physiologic data is reviewed and acted upon outside the clinic—such as blood pressure, glucose, weight, or pulse oximetry—and includes care team work performed to assess trends, communicate with the patient, and adjust the monitoring plan as needed.
CPT 99470 requires at least one real-time, interactive communication with the patient or caregiver during the month and is billed once per calendar month when all requirements are met.
What is CPT Code 99470?
CPT 99470 covers RPM treatment management services performed by clinical staff, a physician, or other qualified healthcare professional. It is billed once per calendar month, as long as:
- The patient is enrolled in an active RPM program
- RPM physiologic data is being collected and transmitted through a qualified device (reported separately under CPT 99454 or CPT 99445)
- The care team performs 10–19 minutes of cumulative RPM treatment management work during the month
- The month includes at least one real-time, interactive communication with the patient or caregiver
This code does not include RPM setup and patient education (reported under CPT 99453), and it does not replace the device supply/transmission codes (CPT 99454 or CPT 99445). Instead, CPT 99470 captures the clinical management work—reviewing RPM data, assessing risk, updating the care plan, and communicating with the patient—when total time falls below the 20-minute threshold required for CPT 99457.
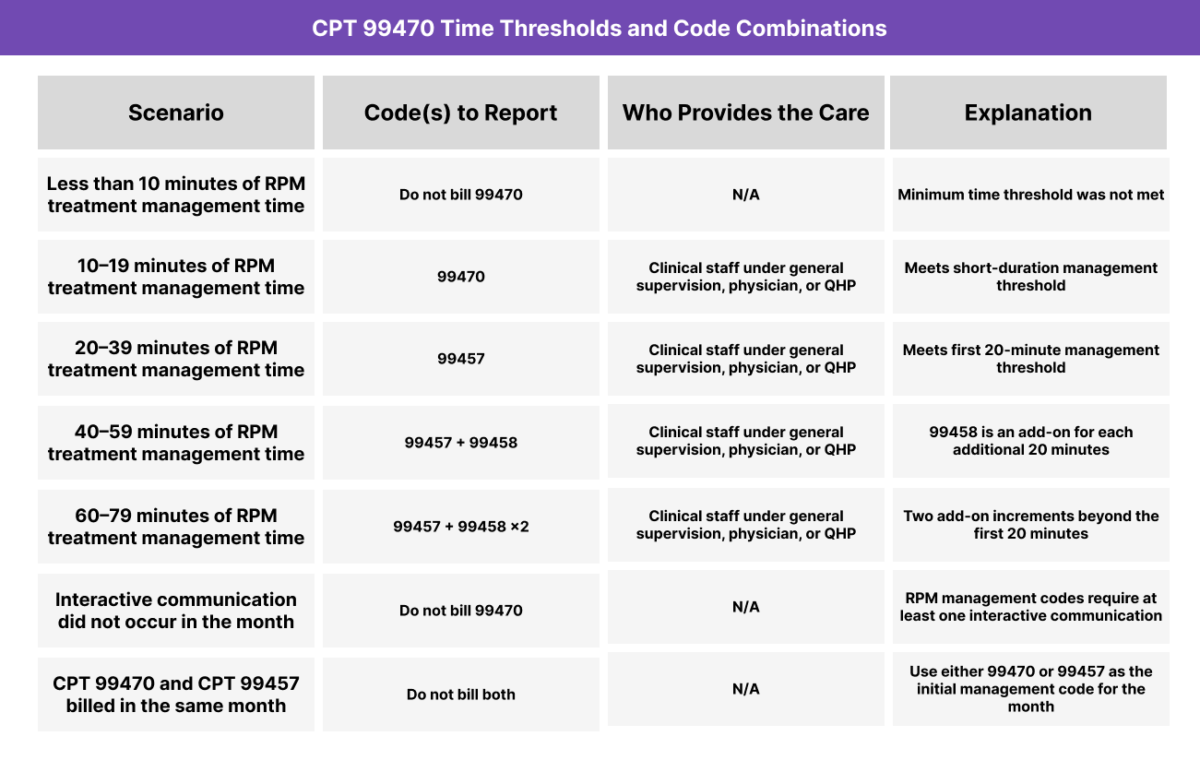
CPT 99470 Time Thresholds and Code Combinations
CPT 99470 may be billed once per calendar month to report RPM treatment management time when the cumulative management work totals 10–19 minutes in the month and includes at least one interactive communication.
Important to Note:
CPT 99470 requires:
- Cumulative RPM treatment management time of 10–19 minutes in the calendar month
- At least one real-time, interactive communication with the patient or caregiver
- Time tracking that reflects work performed by clinical staff, physician, or QHP
- One billing instance per calendar month, per patient
When to Use CPT 99470: Common Scenarios and Use Cases
CPT 99470 is used when RPM data is actively reviewed and managed, but total monthly treatment management time falls between 10 and 19 minutes. It is designed for shorter, clinically meaningful management interactions that still include at least one real-time communication with the patient or caregiver.
Here are examples of how CPT 99470 is used in practice:
CPT 99470: Billing Requirements and Eligibility
CPT 99470 is used to report RPM treatment management services when the care team performs 10–19 minutes of cumulative RPM management work in a calendar month and completes at least one real-time, interactive communication with the patient or caregiver.
It does not include RPM device setup and patient education (CPT 99453) and does not include RPM device supply/transmission (CPT 99454 or CPT 99445). Instead, it captures the clinical work performed to interpret RPM data, contact the patient, and take action based on findings.
Patient Eligibility Criteria
To be eligible for RPM treatment management under CPT 99470, the patient should:
- Be enrolled in an active RPM program with physician/QHP oversight
- Be using a qualified RPM device that transmits physiologic data
- Have an ongoing condition or clinical need that warrants review and management of RPM data
- Common RPM management use cases include:
- Hypertension and cardiovascular risk monitoring
- Diabetes management support
- COPD or respiratory symptom monitoring
- Weight monitoring tied to clinical intervention
- Post-discharge monitoring with clinician follow-up
Service Requirements
To qualify for 99470:
- RPM data must be reviewed and acted upon as part of an ongoing monitoring plan
- Cumulative time must total 10–19 minutes in the calendar month
- The month must include at least one real-time, interactive communication with the patient or caregiver
Time should reflect clinical staff/physician/QHP work such as:
- Reviewing and interpreting RPM data and trends
- Assessing risk and determining next steps
- Adjusting care plans or coordinating follow-up
- Communicating findings and instructions to the patient/caregiver
- Documenting the work performed
Who Can Bill CPT 99470
CPT 99470 may be billed by:
- Physicians
- Nurse Practitioners (NPs)
- Physician Assistants (PAs)
- Other Qualified Healthcare Professionals (QHPs)
Clinical staff may perform portions of the work under general supervision, but billing is tied to the supervising provider.
Billing Frequency and Time Requirements
- CPT 99470 is billed once per calendar month, per patient
- It requires 10–19 minutes of cumulative RPM treatment management time
- At least one interactive communication is required in the month
- If total time reaches 20 minutes or more, CPT 99457 (and 99458 if applicable) should be used instead
CPT 99470 Billing Documentation Checklist
To support compliant billing of CPT 99470, include the following in the patient record:
- A documented RPM order and monitoring plan:
- Clinical rationale for RPM treatment management
- Type of physiologic data being monitored (e.g., BP, weight, glucose)
Evidence the patient is actively enrolled in RPM:
- Device supply/transmission process documented via the appropriate code(s) (e.g., 99454 or 99445)
- Confirmation RPM data was available for review during the month
Cumulative monthly time tracking:
- Total RPM treatment management time of 10–19 minutes in the calendar month
- Notes should reflect what work was performed (not just time totals)
- Optional: time log summaries or platform-generated activity records
Interactive communication documentation:
- At least one real-time phone/video interaction with the patient or caregiver
- Date/time and summary of what was discussed and decided
- Clinical decision-making and follow-up actions:
- Any care plan changes, medication adjustments, escalation, or follow-up scheduling
- Documentation linking actions to RPM findings
Supervising provider identification:
- Claim billed under a physician or QHP
- Clinical staff involvement documented under general supervision
Attestation that:
- Only one unit of CPT 99470 is billed per calendar month
- The RPM management service was not duplicated by another provider for the same patient and month
- CPT 99470 was not billed concurrently with CPT 99457 for the same month
Common CPT 99470 Billing Mistakes (and How to Avoid Them)
❌ Billing With Fewer Than 10 Minutes of Total Time
CPT 99470 requires at least 10 minutes of cumulative RPM management time in the calendar month. If total time is below the threshold, the service is not billable under 99470.
❌ No Interactive Communication Documented
RPM management codes require at least one real-time, interactive communication with the patient or caregiver during the month. Without documentation of that communication, CPT 99470 should not be billed.
❌ Billing CPT 99470 and CPT 99457 in the Same Month
CPT 99470 is intended for months with 10–19 minutes of management time. If time reaches 20 minutes or more, CPT 99457 should be billed instead—these codes should not be reported together for the same month.
❌ Time Logged Without Describing the Work Performed
Time alone is not enough. Documentation should describe the RPM data reviewed, the clinical assessment, patient communication, and any actions taken.
❌ Counting Non-Clinical or Administrative Time
Only time spent on qualifying RPM treatment management activities should be counted. Purely administrative tasks should not be included in billable time.
❌ Submitting More Than One 99470 Per Month
CPT 99470 is billed once per calendar month per patient. Multiple submissions in the same month are not permitted.



