What is a DRG (Diagnosis Related Group?)
Diagnosis-Related Groups (DRGs) are a hospital payment classification system Medicare uses to group inpatient stays into categories that reflect similar clinical conditions and expected resource use. Under the Inpatient Prospective Payment System (IPPS), every inpatient discharge is assigned to a DRG based on the patient’s principal diagnosis, secondary diagnoses, procedures performed, and other factors such as age and discharge status.
DRGs are designed to set a predetermined payment amount for an entire inpatient stay rather than paying separately for every service provided. Each DRG has a “relative weight” that represents the expected costliness of treating patients in that group, and Medicare payment rates are adjusted using these weights.
Today, Medicare uses Medicare Severity DRGs (MS-DRGs), which refine the original DRG model by accounting for complication and comorbidity severity. MS-DRGs help differentiate higher-acuity cases from more routine stays so payment better matches expected resources.
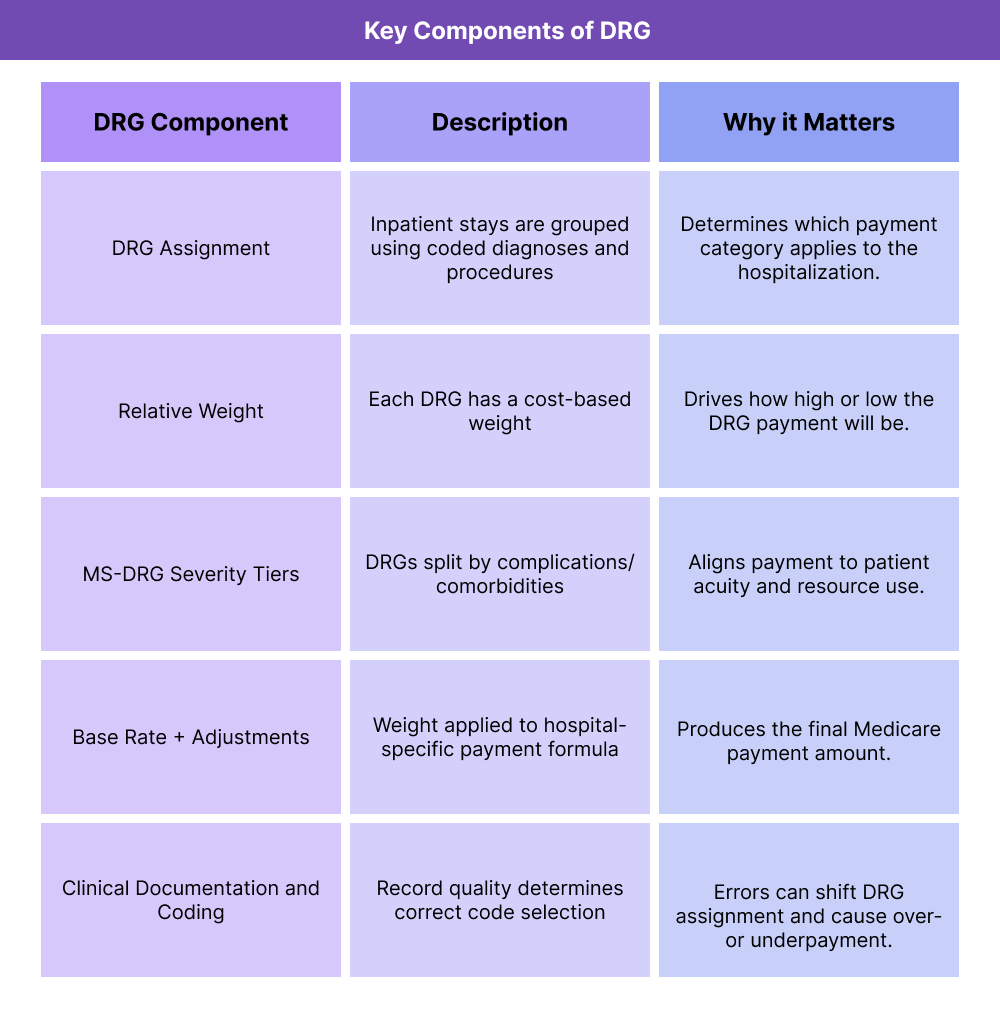
Key Components of DRG
DRGs are designed to translate complex inpatient hospital care into standardized payment categories. CMS assigns each inpatient stay to a DRG using diagnosis and procedure coding, and then uses that DRG to determine a bundled payment amount for the hospitalization.
Although DRGs are often discussed as a single system, there are core elements that explain how they work and why different DRG types exist.
DRG Assignment Based on Clinical Coding
Every inpatient discharge is grouped into a DRG using information from the medical record that is translated into ICD-10 diagnosis and procedure codes. The grouping logic considers the principal diagnosis, any relevant procedures, and secondary diagnoses that add complexity.
Accurate clinical documentation and coding are essential because DRGs are only as correct as the coded record behind them.
Relative Weights and Expected Resource Use
Each DRG has a relative weight that reflects the expected cost of treating patients in that category. Higher-weight DRGs represent more complex cases that use more hospital resources, while lower-weight DRGs represent routine stays. Medicare uses these weights to scale payment up or down.
Medicare Severity DRGs (MS-DRGs)
Medicare uses MS-DRGs, which divide many DRGs into severity tiers based on whether the patient has complications or comorbidities. This ensures that a higher-acuity version of a condition is paid differently than a lower-acuity one.
Geographic and Hospital-Specific Adjustments
DRG weights are applied to a base payment rate that is adjusted for factors such as wage index and hospital characteristics. These adjustments help align DRG payments with local cost conditions and facility role.
How DRGs Work in Practice
DRGs operate as the practical mechanism Medicare uses to pay hospitals for inpatient stays under a bundled, prospective model. Instead of paying line-by-line for each service delivered during a hospitalization, Medicare assigns the entire stay to a DRG and pays a set amount based on that classification.
Step 1: Clinical Care Is Documented During the Inpatient Stay
Throughout the hospitalization, clinicians document the patient’s conditions, treatments, procedures, and clinical course. This documentation becomes the source record that determines what diagnoses and procedures can be coded after discharge.
Step 2: Coders Translate the Record Into ICD-10 Codes
After discharge, coding teams assign ICD-10 diagnosis codes and procedure codes based on the documented record. The principal diagnosis, secondary diagnoses, and any procedures are all captured at this stage.
The quality and specificity of documentation directly shape how accurate the coded record will be.
Step 3: The Case Is Grouped Into a DRG (or MS-DRG)
Once coding is complete, the case runs through a grouper that assigns the stay to a DRG. Under Medicare, this is an MS-DRG, which accounts for severity by placing the case into a higher or lower tier depending on documented complications and comorbidities.
Step 4: Payment Is Determined From the DRG Weight
The assigned DRG has a relative weight that reflects expected resource use. Medicare applies that weight to its inpatient payment formula to determine the bundled reimbursement for the stay.
If DRG assignment changes, payment changes with it.
DRG in Billing, Reimbursement, and System Limitations
DRGs are a core Medicare inpatient billing mechanism because they determine how hospitals are paid for most acute inpatient stays. Under the Inpatient Prospective Payment System (IPPS), DRGs create a bundled, fixed payment amount for the entire hospitalization, regardless of how many individual services were delivered. This shifts payment focus from volume of services to the clinical classification and severity of the case.
How DRGs Drive Inpatient Reimbursement
Once an inpatient stay is grouped into a DRG or MS-DRG, Medicare calculates payment using:
- The DRG’s relative weight
- A standardized base payment rate
- Hospital-specific adjustments (such as labor cost differences and facility factors)
Higher-weight DRGs pay more because they represent more complex stays with higher expected resource use. Lower-weight DRGs pay less because they represent routine, lower-acuity hospitalizations. Even small shifts in coding that change DRG assignment can materially change reimbursement.
DRGs, MS-DRGs, and Case Mix Index
Medicare uses MS-DRGs to adjust payment based on severity. This means the presence of documented complications or comorbidities can move a case into a higher-severity MS-DRG with a higher payment weight.
DRG patterns across a hospital also shape the case mix index, which is a measure of how clinically complex a facility’s inpatient population is. A higher case mix index generally correlates with higher overall inpatient reimbursement because it reflects a heavier concentration of high-severity DRGs.
System Limitations and Operational Watch-Outs
DRG payment depends entirely on the coded discharge record, which introduces predictable limitations:
- DRGs reflect documented severity, not necessarily true clinical severity if documentation is incomplete
- Coding quality and timing can affect DRG assignment and delay final billing
- DRG logic is complex and can be misapplied when documentation is vague or inconsistent
- Hospitals may experience underpayment if complications/comorbidities are not captured clearly in the record
For healthcare SaaS buyers, DRGs highlight why inpatient documentation quality, clinical specificity, and coder-aligned workflows are financially critical.
How DRGs Influence Quality, Access, and Equity in Healthcare
Although DRGs are payment tools, they shape care delivery by influencing hospital incentives, resource allocation, and performance priorities. Because DRG reimbursement is fixed per case, hospitals are motivated to manage length of stay, reduce avoidable complications, and deliver efficient care that aligns with expected resource use.
Quality and Safety Effects of DRG Payment
DRGs encourage hospitals to reduce preventable complications and inefficiencies. If complications occur or care is poorly coordinated, hospitals often incur additional costs without receiving additional payment, since DRGs are bundled.
This creates system-level incentives to strengthen:
- Early complication detection and prevention
- Efficient discharge planning and transition workflows
- Clinical documentation accuracy that supports appropriate DRG placement
- Consistent inpatient care standards that reduce avoidable variation
In combination with quality programs layered on top of inpatient payment, DRGs reinforce the operational value of safer, more standardized inpatient care.
Access Implications in Inpatient Care
Because DRGs standardize payment, they can indirectly affect access to certain inpatient services. Hospitals may prioritize programs and care pathways that can be delivered within expected DRG resource thresholds, while high-cost cases can create financial strain.
When DRG rates do not fully align with real-world costs, hospitals may face pressure that influences:
- Availability of specialized inpatient services
- Staffing levels for high-acuity units
- Investment in inpatient care coordination support
A well-calibrated DRG environment supports stable inpatient access; misalignment can create service pressure in resource-heavy cases.
Equity Considerations Under DRG Systems
Fixed DRG payment can produce equity challenges when patient populations have higher clinical complexity that is not fully captured through documentation or coding. Facilities serving more medically complex, socially vulnerable, or safety-net populations may experience higher costs per DRG than reimbursement reflects.
Equity-sensitive DRG performance depends on:
- Accurate documentation that captures true severity
- Care coordination models that reduce avoidable escalation
- System supports that prevent underpayment driven by incomplete records
In this way, DRGs make documentation accuracy and severity capture not just a revenue issue, but an equity and access issue for hospitals serving high-risk populations.
Frequently Asked Questions about DRGs
1. What are DRGs (Diagnosis-Related Groups)?
DRGs (Diagnosis-Related Groups) are inpatient hospital payment categories that group stays with similar clinical conditions and expected resource use to determine a bundled Medicare payment amount.
2. What is the difference between a DRG and an MS-DRG?
A DRG is the general payment grouping category. An MS-DRG (Medicare Severity DRG) is Medicare’s version that splits many DRGs into severity tiers based on documented complications or comorbidities, so higher-acuity cases are paid more.
3. How are DRGs assigned?
DRGs are assigned after discharge using ICD-10 diagnosis and procedure codes from the medical record. The principal diagnosis, secondary diagnoses, procedures, age, and discharge status all influence grouping.
4. Why do DRGs matter for hospital reimbursement?
DRGs determine the fixed, bundled payment Medicare pays for an inpatient stay under IPPS. The assigned DRG’s relative weight drives how high or low the payment will be.
5. What is a DRG relative weight?
A DRG relative weight represents the expected costliness of treating patients in that DRG. Higher weights indicate more complex, resource-intensive stays and lead to higher reimbursement.
6. What is case mix index and how does it relate to DRGs?
Case mix index is a hospital-level measure of overall inpatient clinical complexity derived from DRG weights. A higher case mix index typically reflects a higher-acuity patient population and higher aggregate inpatient reimbursement.
7. Can documentation affect DRG payment?
Yes. DRGs depend on the coded record, so incomplete or nonspecific clinical documentation can lead to lower-severity DRG assignment and underpayment, even if the patient was clinically complex.
